Let Me Tell You About That Time My Daughter Was On Medicaid
Health care. Unless you live in a cave without Wi-Fi, you’ve heard the familiar rumblings of our elected officials holding the fate of every American citizen in their hands while they decide what to do about it. I have a lot of thoughts about how something that impacts so many could be determined by 13 white men in DC (and yes, the fact that they are white men is relevant and worth noting), a lot of thoughts, but instead, I will share the story of my daughter being a Medicaid recipient.
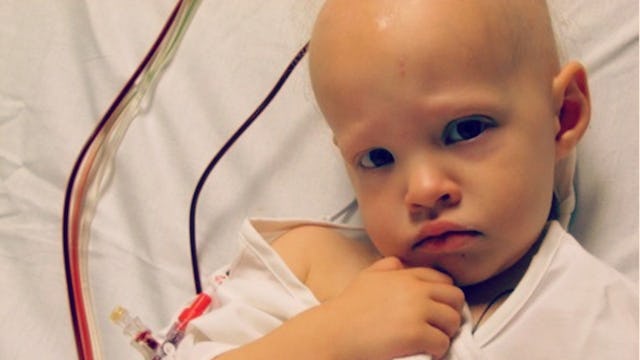
Once upon a time, March 23, 2007, to be precise, my not-quite-2-year-old daughter Donna was diagnosed with a brain tumor. My husband and I both worked at the time, he at a job he had been at for five years and me at a job I had been at for nine years. I was thrilled to be able to transition to part-time hours after my girl was born and felt lucky most every day. Our family benefited from generous employer-provided benefits.
I needed to exit my position when it became clear that the care our girl would require would prevent me from being available to work on any consistent basis. After diagnosis and her initial surgery to remove the tumor, our girl relapsed six weeks later. That resulted in another hastily scheduled brain surgery and the need for chemotherapy that would require hospital stays of 3–7 days, twice monthly, for an unspecified time. We needed to tighten our belts a bit, but we could and did.
Many cancers are understood adequately enough to follow a treatment protocol. If you have a boy with leukemia, you know that he will be in treatment for 3–3 1/2 years. A dear friend who cares for a daughter with a brain tumor learned a couple of years post-diagnosis that her girl would need to receive a new regimen of chemotherapy once a week for 52 weeks. Now, none of these protocols are set in stone, as at any time, something could happen that would require changes — the cancer could return, metastasize, infection could set in, the chemo could stop working.
For the cancer my daughter had, papillary meningioma, no such treatment protocol exists. Not enough research has been done to understand it — actually, nothing more than anecdotal studies have been published about this particular type of brain cancer and no research or funds are devoted to better understanding it. As the docs explained, that was both good and bad. Bad because, well, there was no plan, and good because, well, they could try what they had and hope for the best, as nothing out there suggested it would not work. Donna’s doctors chose hope, and we did too.
Initially, Donna’s cancer responded to treatment incredibly well. Lesions in her lungs were erased (Donna’s cancer had metastasized) and there was no sign of any returning tumor growth in her brain. The joy and relief we felt compensated for the days of suffering Donna experienced using a chemo cocktail an oncologist friend described as a “sledgehammer.”
Each cycle required a five-day inpatient stay followed by discharge to home followed by the onset of neutropenia followed by a second monthly hospitalization for IV antibiotics to combat any chance of infection setting in and wreaking havoc. Two weeks of the month were spent inpatient, one week spent post-chemo feeling like hell, and one blessed week a month where we could enjoy relative good health and engage in things 2-year-olds like to do — parks, zoo, playing outside.
We did this for six months, not knowing month to month if we would keep doing it, as we never knew if it would stop working or if it would become too toxic. After six months, it did. Donna’s kidneys began to fail, hit particularly hard by the chemo. The treatment team advised she stop the protocol, extract healthy cells via harvest, then have a stem cell transplant (or two, depending on whether or not she survived the first, and no, I am not joking) to provide what they hoped would be the final blow to her cancer.
A stem cell transplant is to chemo what a marathon is to a 5K.
All of this happened prior to the Affordable Care Act and an Obama presidency. My husband and I, despite being grateful for the insurance we had, were running a silent tally in our heads. Each hospital stay came with a cha-ching! echoing in our heads. Each home health visit to access her port, each surgery, each pink plastic bowl used to catch toxic vomit was adding up. It was a pressure we lived with but didn’t share. The health of our girl was consuming, so we back-burnered the worry of Donna’s $2 million lifetime insurance cap, but knew we were inching closer to it every day.
In a collective fog, we marched toward Donna’s stem cell transplant, only to come to a screeching halt when it was denied by our insurance carrier. In December of 2007, our family was lucky enough to live in a state and in a time that insurance was mandated for children. When our employer provided insurance denied the recommended stem cell transplant and then denied our appeal, the hospital suggested we apply for Medicaid for Donna under Illinois’s All Kids program. They walked our upper-middle class, naïve selves through the process.
Each month, a little slip of paper came in the mail that allowed Donna to access her oncologist-recommended treatment. It was her Medicaid slip that held the particular sequence of letters and numbers that acted as a key to her potential health and well-being. It was used exclusively during the time of her stem cell transplant and recovery, as our insurer made clear nothing related to a stem cell transplant would be eligible for coverage.
Donna’s single stem cell transplant cost well over $600,000. We were grateful that Medicaid covered the transplant for a couple of reasons: 1) simply because it would be paid for without us losing our home or financial stability, and 2) because that $600,000-plus would have taken Donna dangerously close to her $2 million lifetime insurance cap. The short period that Donna was on Medicaid acted as a reprieve to our worries about Donna maxing out her lifetime insurance cap before reaching the age of 3.
I remember the day the Affordable Care Act passed and the day the Supreme Court upheld it. While it no longer impacted our girl who died before it was passed, I celebrated for the hundreds of children and families I knew who lived with pediatric cancer and its devastating impact, both emotional and financial. I celebrated that these kids lucky enough to survive their cancer could never, ever again be denied for having had the misfortune of having a pre-existing condition. I celebrated that they would be allowed to enjoy their parent’s insurance coverage until age 26. I celebrated that they would be relieved of the burden of a lifetime cap. These are good, important measures for quality of life that have nothing to do with whether you vote red or blue.
While Vice President Pence extols the virtues of “personal responsibility” and Kellyanne Conway advises people to get a job with employer-provided benefits rather than rely on Medicaid, too many Americans know the reality of why that approach to health care does not scratch the surface of reality. That approach deems to separate the “deserving” poor from the “undeserving” poor. That approach does not take into account the reality of average Americans living with catastrophic illness, working jobs that do not provide a living wage, let alone health benefits, or the often random nature of illness, unemployment, and falling on hard times. My upper-middle class, white lady, married, respectable, employed self needed and benefited from Medicaid when it covered our daughter after our for-profit insurer denied her.
We are at the cusp of moving backwards on health care in America, dangling over a proverbial cliff that will put so many fellow Americans in harm’s way. Medicaid benefits vulnerable people that you know and love — parents and grandparents in nursing homes, veterans, children, 50% of every baby born here, people living with mental illness, people living with addiction, people living with catastrophic illness not covered by their insurance. You may never have used Medicaid yourself, but you can never claim you will never need it because, well, life.
Call your senators. Today. Now. You can find their number here. Tell them Donna sent you.