What to Expect When Your Baby has a Congenital Heart Defect
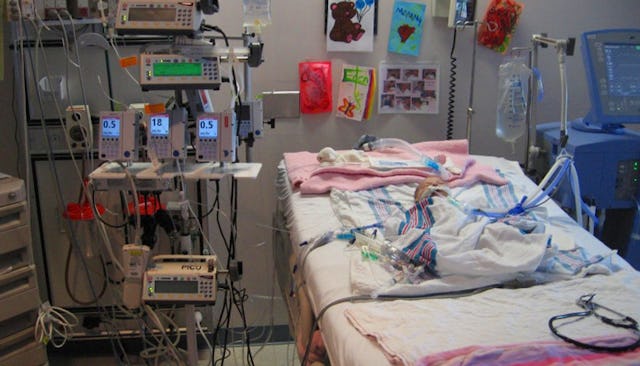
After the harrowing journey of labor and delivery, I was given the kind of news no mother wants to hear- “Your baby has a congenital heart defect (CHD)”. In my case, Eden was born with Transposition of the Great Arteries- a defect that without immediate surgery, would end in death. So without any preparation or warning, I was thrown into the world of cardiologists and intensive care units. My baby was whisked out of my arms and instead of her first bath, first nursing session and first poop, she was placed in the care of doctors and nurses to suffer through endless poking and prodding. They tried to explain to me what was happening to her, but I couldn’t grasp the enormity of the situation. I didn’t understand about prostaglandin hormones and central lines, I just wanted to know what to expect- in laymen’s terms.
You might be in the same situation. Here is the kind of realistic advice I needed during those first few days:
1. It will take one or two nurses to get your baby in your arms. Every new mom wants to hold and snuggle her infant. A baby with a CHD (prior) to surgery will have several wires attached to her. Expect a central line going through the site of the umbilical cord, as well as other IV lines in her hands or feet, plus all the wires used to monitor her vitals. When you think you want to hold your child, make sure you have gone to the bathroom, had a snack, and are in a comfortable position. Once she is moved into your arms, moving her back to the bed won’t be simple.
2. Nursing may not be an option.The nurses in the PICU might encourage you to nurse her if you planned to breastfeed. If you try, do not get discouraged if it isn’t a feasible option. The lines to contend with, plus a CHD baby’s labored breathing might make breastfeeding stressful. Your baby may be on a breathing machine (CPAP or a ventilator) both of which make nursing impossible. Even if you are unable to breastfeed prior to surgery, you will be able to try again when she is better. I didn’t start nursing Eden until she was six weeks old. We managed to wean off the bottle and she breastfed for two years. Don’t give up hope and don’t beat yourself up if it doesn’t work. You and your baby have enough to worry about — feeding should be as stress free as possible.
3. Expect a fussy baby. This seems like an obvious observation, but there are other reasons besides wires that are making your baby fussy. Some infants are given a hormone called prostaglandin. All infants are born with a small hole in their heart that closes up after a few days. For children with the type of defect Eden had, the prostaglandin is given to keep that hole open, so enough oxygenated blood will get distributed throughout the body until the surgery corrects the problem. This hormone causes fever and irritability. Another reason for fussiness? Since there are so many procedures to be performed, infants with CHD cannot be swaddled, a common soothing technique. If you want to simulate that experience, try gently pressing in on either arm of your child with your hands. Subduing her limbs with a bit of pressure can simulate the feeling of being swaddled.
4. A spinal tap might be necessary prior to surgery. Most parents cringe when they hear the phrase “spinal tap” as it is associated with pain and trauma. Since your child is about to have open-heart surgery, doctors will want to ensure that your baby is healthy enough for the operation. A spinal tap is used to test for infection and meningitis, and is often standard procedure prior to major surgery.
5. Try to get some rest prior to “operation” day. The thought of leaving your baby in the PICU without you is hard to imagine, but you will be better able to help your child recover if you are rested. Find a friend or parent to stay with your baby overnight and go home and get some rest. You will want to have energy for those post-op recovery days. Your baby might be on a mild sedative like Ativan, and won’t be awake enough to miss you.
6. Expect ups and downs. Every day in the PICU is harrowing. Monitors beep the minute a vital sign dips below normal range, and you may find yourself going crazy watching all those numbers. Keep in mind that “normal” ranges are not applicable to your child. While a healthy newborn should have O2 of 95 or higher, babies with CHD’s have O2 levels in the high 70’s and 80’s. This is to be expected. The brain is the last organ to be deprived of oxygen so you should not worry about brain damage. In some cases, doctors want the O2 level to stay below normal so it doesn’t put extra pressure on a sick heart.
7. Visitors will be limited. As is policy with most intensive care units, the ability to have visitors will be limited to family only. In the winter months, many hospitals will not even allow children under twelve due to the high instances of cold and flu. If you have other children at home who are unable to visit prior to the operation, bring home pictures and video of your little one so they can feel a part of the baby’s life.
8. Remind yourself that many congenital heart defects are correctable. As surgery approaches, practice deep breathing and meditation. Have others bring meals and do housework for you. Keep this fact in your head: Lots of children survive and thrive after heart surgery.
Eden is now seven years old and I go months forgetting she was born with such a severe defect. Those days may seem decades away, but it will happen; the trauma of pregnancy, birth, and a sick baby won’t last forever.
This article was originally published on