Figure Out Your Breast Cancer Risk, And What To Do About It
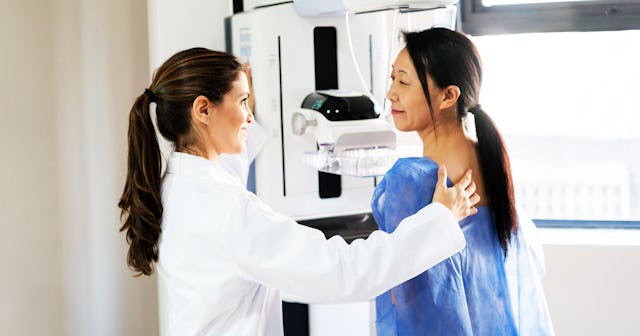
I was 35 years old when I was diagnosed with breast cancer. I didn’t have a family history, so I figured I shouldn’t be too worried. After all, this was my third breast lump in ten years, and the first two were harmless masses. Why would this one, found during my self exam, be any different?
It turns out, I was at risk of breast cancer and I simply didn’t know it. I’ve spent the past four years, since my diagnosis, educating others by sharing my story. I was young, active, ate a healthy diet, and went to my gynecologist yearly for a clinical breast exam and pap smear. How did I end up being part of the one in eight women diagnosed with invasive breast cancer? It’s critically important that you understand your breast cancer risk.
I interviewed Dr. Anjali Malik, a breast radiologist, to get all the important info we need to know, right now, about our breasts and how to keep them healthy. For starters, we always preach that women need to know their risk of breast cancer, but what does that mean? How do we figure out our breast cancer risk, and once identified, what do we do about it?
Dr. Malik explains that women have both “nonmodifiable and modifiable risk factors for the development of breast cancer.” She wants us to understand both, because some risks can’t be changed, while others can. Furthermore, she wants women to figure out — early on — if they need to be monitored for breast cancer prior to age forty. She shares that a “formal risk algorithmic calculation” is possible — with the help of a qualified doctor.
I know. Sometimes we just don’t want to know. What we don’t know can’t hurt us, right? Wrong. Knowing our risk factor can actually be empowering. Instead of waiting to see if cancer chooses us or not, we can know our bodies, be proactive in getting exams and scans, do self-exams, and potentially engage in genetic testing for not only our benefit, but the benefit of our biological relatives. Plus, we can work on those modifiable risk factors that Dr. Malik warned us about.
There are several risk factors for breast cancer. The top two, according to Dr. Malik, are aging and being female at any point. She adds that this means a cisgender woman, transgender man who underwent puberty as a woman, or transgender man on hormones. One of the nonmodifiable factors that puts someone at risk of breast cancer, she says, is family history of premenopausal breast cancer, a known genetic mutation, family history of male breast cancer. Someone who is Black or of Ashkenazi Jewish descent, someone who has a “history of large doses of chest radiation,” started their period earlier than age 12, or started menopause after age 55 are also at a greater risk.
Alright, I know that sounds scary, but there is some hope. There are three major, modifiable breast cancer risk factors. The first is limiting alcohol consumption. Another modifiable risk factor is weight. Dr. Malik shares that “maintaining a healthy weight” reduces risk. Finally, exercise can reduce risk. Dr. Malik shares that the American Cancer Society advocates for “150 minutes per week of moderate to strenuous exercise.” Interestingly, these three factors play into one another. Less alcohol, keeping our weight in check, and exercising all have many health benefits, including reducing breast cancer risk.
Though oral contraceptives and hormone replacement therapies are popular, Dr. Malik emphasizes the importance of discussing these with your doctor. Of course, there are benefits, but “they must be weighted against your level of personal risk.” This is another modifiable risk factor that a patient can take into their own hands.
I asked Dr. Malik about those modifiable factors — lifestyle changes — that are recommended. Do they really make a difference in our breast cancer risk? She shares, “I think all of those changes would affect more than just breast cancer risk! Given that we are all at risk of at least 1/8, I think taking every measure to reduce our risk is important.”
What if you find out that your risk is higher than the average woman? What are you supposed to do? Dr. Malik wants you to talk to your doctor. Also, be aware that “75% of those who develop breast cancer have no family history, and only 5-15% of breast cancers are genetic.” Most women who develop breast cancer, she notes, do not have a genetic component.
As a mom of four adoptees, I wanted to know what people who were adopted or those who only have one biological parent in the picture supposed to do to learn their risk. After all, many people don’t have information about all or some of their biological family. Dr. Malik points these individuals to a genetic counselor who can help the person figure out whether genetic testing is the right course for them. She also recommends contacting the agencies that assisted with the egg, sperm, embryo donation or the adoption to see if medical records can be obtained.
If you are at a high risk of developing breast cancer, there are options. Dr. Malik encourages “earlier screening protocols, more frequent screening or utilizing MRI in addition to mammograms, and if genetics warrant it, early family planning and fertility preservation through egg freezing.”
As a two-time breast cancer survivor, I often tell others that early detection truly does save lives. Dr. Malik agrees. “I once had a patient who reconnected with her biological family and discovered a strong family history of breast cancer.” This patient received genetic testing, found out she had a genetic mutation, and had an MRI. The results? She learned she had a very small, early stage breast cancer. By taking a proactive approach to her health, the patient was saved. “We want to empower you into action, not anxiety,” Dr. Malik says.
Certainly, it seems like some patients — like me — simply shouldn’t have breast cancer. Yet the reality is, I had it — twice — and breast cancer is discouragingly common in women. However, as we learn more and more about what causes cancer and what also redeems us from it, I am thankful for modern medicine and the hard-working medical professionals like Dr. Malik. Knowing your risk, staying in communication with your doctor, and getting checked may save your life.
This article was originally published on