Living With ME/CFS Is Hell, And Many COVID Longhaulers Are Experiencing It
It’s been more than a year since the very first case of COVID-19 was contracted in Hubei province in China. Since those very early days, the virus has gone on to infect more than 57 million people worldwide, with more than 11 million of those cases happening in the United States (as of this writing). Many have survived and more than one million have died worldwide. It’s a devastating loss, a steep price.
But to write the story of COVID-19 in terms of life or death, survival or not, would be to ignore the growing number of survivors’ voice demanding to be heard. An untold numbers of folks known as COVID Longhaulers have survived, but have been plagued with ongoing, chronic, debilitating symptoms that make it impossible to return to their normal lives.
To add more uncertainty to the actual toll of COVID-19 on us all, even among COVID Longhaulers, the outcome is not uniform. Some longhaulers experience ongoing symptoms, such as fever and cough, others are experiencing organ damage, and yet another subset are developing myalgic encephalomyelitis/chronic fatigue syndrome, ME/CFS for short.
During a news conference on COVID-19 organized by the International AIDS Society, Dr. Anthony Fauci, Director of the National Institute of Allergy and Infectious Diseases and member of the White House Coronavirus Task Force, highlighted the link between COVID-19 and ME/CFS. He said, “[Y]ou can see people who’ve recovered who really do not get back to normal that they have things that are highly suggestive of myalgic encephalomyelitis and chronic fatigue syndrome. Brain fog, fatigue, and difficulty in concentrating so this is something we really need to seriously look at because it very well might be a post-viral syndrome associated with COVID-19.”
What is ME/CFS?
“ME/CFS is a multi-system disease that causes profound metabolic dysfunction and is accompanied by physical and cognitive limitations,” according to #MEAction Network, an international ME/CFS advocacy group.
The CDC describes ME/CFS as “a disabling and complex illness.” The disease renders folks unable to do their usual activities due to debilitating exhaustion known as post-exertional malaise (PEM), which is more intense than the kind of fatigue you might feel after a long day. It is not improved by rest, and may even get worse after activity—physical or mental activity.
Jaime Seltzer, #MEAction Director of Scientific and Medical Outreach, writes “PEM does not feel like fatigue or the usual uncomfortable burn you get from going back to the gym after a long time away. It is a unique experience, and in its most extreme forms feels like descriptions of shock and hypoxia more than weariness.”
Other symptoms of ME/CFS may include sleep troubles, issues with concentration and thinking, pain, and dizziness.
The CDC notes that “[p]eople with ME/CFS are not able to function the same way they did before they became ill,” and “ME/CFS often makes it hard to keep a job, go to school, and take part in family and social life.”
ME/CFS affects all races, genders, and ages, but women and adults between 40 and 60 years old are most likely to be affected. Seltzer also emphasizes that “[w]hile the diagnosis is often made in white people, studies show that incidence in BIPOC populations is just as high if not a little higher.”
The link between COVID-19 and ME/CFS
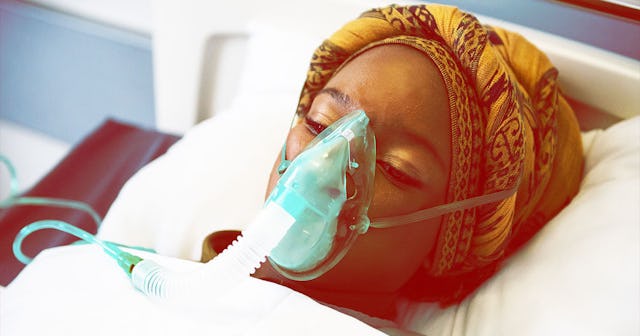
Nitat Termmee/Getty
Experts expect that at least 10-12 percent of all people with COVID-19 will go on to develop ME/CFS, which often develops after a viral infection, though may be triggered for other reasons.
Experts don’t know exactly why this condition develops in some subset of folks even after the virus has been eradicated from the body. One theory put forth by Dr. Anthony Komaroff, a physician at Brigham and Women’s Hospital in Boston who has treated ME/CFS patients since the 1980s, is that ME/CFS might be traced back to the brain. The center in the brain that activates when you’re sick may not turn off.
The struggle for diagnosis
Seltzer notes that “there is no single lab test that provides a definitive diagnosis. Because of this, the diagnosis is made based off of symptom-based diagnostic criteria.” The Canadian Consensus Criteria (CCC), an international criteria, is a diagnostic tool frequently used by researchers and clinicians.
Many COVID longhaulers are finding it difficult to receive a ME/CFS diagnosis because many medical providers are not educated about ME/CFS or doctors attempt to rule out all other diagnoses first before landing on a result of ME/CFS.
The delay may be particularly damaging for ME/CFS patients. For example, where gradual exercise may be good for some COVID longhaulers, exercise can be particularly harmful for COVID longhaulers suffering from ME/CFS. In fact within the last few years, the CDC revised its guidelines for ME/CFS and acknowledged exercise may make the disease worse.
What can ME/CFS patients expect?
There is no cure for ME/CFS. More research is needed into the hows, whys, and treatments of this disease.
Seltzer writes that, “The first several months are almost always most severe; but the majority of adult patients slowly climb up to a state of better well-being in the 9 mo – 2 year frame. People who ride out this time with caution, do not overdo it, and take careful care of themselves will very often find that the worst is over in less than a year.”
However, complete recovery is rare, and most will be sick, though less sick than they were initially, according to Seltzer. She distinguishes between the “acute” phase of illness and the “chronic” phase. It is likely that patients will have learned how to manage the disease, and will be able to live a good life, though likely different than the one they’d imagined.
ME/CFS patients are encouraged to rest in the early stages of disease and then to pace when able. An enforced period of rest at the onset of symptoms resulted in the best prognosis, according to an expert clinician. Pacing is a strategy wherein patients are active when able, rest when tired, and even plan extra rest ahead of more strenuous activities. (#MEAction offers a pacing guide for patients.)
Julie Rehmeyer, Jennifer Brea and Brian Vastag, in an article for the Washington Post offer these tips for patients suffering from any persistent symptoms:
- Trust your body. Rest when you need to rest. Exercise, even gradual exercise, may make the symptoms worse.
- Ignore those who are telling you that your symptoms are only in your head. They suggest looking “for a therapist who has experience with chronic illness and who will believe and support you, and protect yourself from anyone who doubts the reality of your illness.”
- “Don’t expect doctors to have all the answers.” Doctors are one resource. Another may be support groups and fellow patients.
The more we learn about COVID-19, the more we are realizing that there are not only two outcomes to this disease. It is not the case that you will either survive or perish. In between life and death, survival and not, there’s an entire spectrum of outcomes, including the possibility of developing ME/CFS.
Vaccines are coming. There is a light at the end of this dark tunnel we’ve been trapped in for way too long. But until then it’s so important to remember that COVID-19 is real and serious and that we don’t yet know all there is to know about the long-term consequences of contracting this disease. Until we do know, please social distance, wash hands, and wear a mask.
Information about COVID-19 is rapidly changing, and Scary Mommy is committed to providing the most recent data in our coverage. With news being updated so frequently, some of the information in this story may have changed after publication. For this reason, we are encouraging readers to use online resources from local public health departments, the Centers for Disease Control, and the World Health Organization to remain as informed as possible.
This article was originally published on