What To Know About COVID Vaccines And Allergic Reactions
I don’t know about you, but to me, one of the scariest things to come out of 2020 has been having to embrace the unknown.
The unknown of a wannabe dictator who may or may not refuse to abdicate his throne.
The unknown of a disease that seemed to come out of nowhere, quickly dismantling our entire way of life.
And now the unknown of a vaccine that may feel rushed and new to some, but is actually decades of research in the making.
All of these unknowns, combined with how completely insane 2020 has turned out to be, have put people understandably on edge. So it’s fair to say that none of us feel good hearing about serious allergic reactions to the vaccine.
But here’s the good news: allergic reactions are not entirely unheard of with vaccinations, they can be treated, and there are already safeguards in place to keep all patients receiving the COVID-19 vaccination safe.
The Centers for Disease Control (CDC) classifies adverse vaccine reactions in three ways:
- Local: This is the most commonly reported (and least severe) type of vaccine reaction and may be as simple as redness at the injection site
- Systemic: This might be a fever, and is less commonly reported than local reactions
- Allergic: This is the least commonly reported type of reaction
Severe allergic reactions (think: anaphylaxis) to vaccines are considered extremely rare, but they do happen. This is why young children are typically asked to remain in their pediatrician’s office for 15 to 30 minutes after their initial vaccines to monitor for any signs of an allergic reaction. Some families with a history of severe allergic vaccine reactions are even encouraged to opt out of future vaccinations, just to be safe.
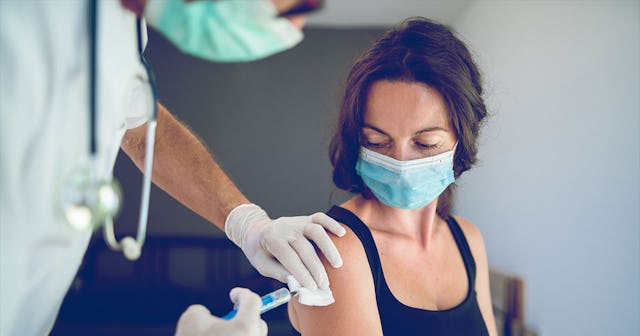
SDI Productions/Getty
But again, these types of reactions are extremely rare.
When they do happen, they can be treated in a medical setting. In fact, the vast majority of patients who experience anaphylaxis go on to fully recover when treated quickly.
It is for this reason that the CDC began preparing for potential anaphylaxis reactions to the COVID-19 vaccine early on, and why current recommendations and safeguards include:
- Talking to your doctor about any severe allergic reactions you’ve had in the past—if you’ve had a severe allergic reaction to other vaccines, or ingredients in the COVID-19 vaccine, you will need to decide together whether or not it is safe for you to get this vaccine
- If you have a severe allergic reaction to the first dose of the COVID-19 vaccination, you should not get the second dose
- All patients who receive the vaccination should be monitored on site for 15 minutes after receiving the vaccination, for 30 minutes if they have experienced previous severe allergic reactions
- All medical providers administering the vaccine should have appropriate medications and equipment on hand for treating severe allergic reactions
- Rapid care should be provided to any patient who exhibits signs of a severe allergic reaction
These guidelines have been put into place specifically to quickly identify and treat any allergic reactions to the COVID-19 vaccination. But again, most of us don’t have to worry about this—especially if you’ve never experienced a severe allergic reaction before. These types of reactions are extremely rare. And the fact that they can so quickly be treated means that the risk of an allergic reaction to the COVID-19 vaccination is nothing compared to the risks of contracting the disease.
So get your vaccination when it becomes available to you, talk to your medical practitioner about any concerns you may have, and remain seated for 15 to 30 minutes after your vaccine to be monitored—just in case.
Assuming you are among the majority of people who won’t experience an allergic reaction, return for your second dose when your doctor tells you to and then breathe a sigh of relief.
Because vaccines really are a miracle, and in this year of unknowns the one thing we should all be well-aware of is how lucky we are to live in a time when vaccines exist.
We may actually have the hope of returning to “normal” sometime in the very near future because of them. And that is something worth celebrating.
Information about COVID-19 is rapidly changing, and Scary Mommy is committed to providing the most recent data in our coverage. With news being updated so frequently, some of the information in this story may have changed after publication. For this reason, we are encouraging readers to use online resources from local public health departments, the Centers for Disease Control, and the World Health Organization to remain as informed as possible.
This article was originally published on