Hospitals May Soon Be Forced To Ration Care, And This Is A Dire Warning
Few moments shake you to your motherhood core like rushing your child to the ER. As a parent to an asthmatic child, I’ve done it twice, holding my son in my arms as he gasped for breath. Watching as his lips started to turn blue and he went limp in my arms. Desperate for the steroid that I knew would reopen his airways.
And it’s because of those frantic hospital visits that I’m particularly concerned when I hear stories about hospitals running out of beds and finding themselves understaffed as COVID-19 rages on. I know what it feels like to have a loved one need one of those beds. And need a doctor’s help to be able to breathe again.
Yet, because Americans continue their refusal to make even the smallest of sacrifices, and instead still gather in groups to watch football (mask-less), host birthday parties (mask-less), and deny the existence of a virus that’s killed 1.3 million people around the world, that’s exactly what is happening in hospitals across our nation.
Doctors and nurses are imploring us, as they work tirelessly to fight this beast, to listen to them.
They are running out of beds.
They are running out of staff.
They are running out of supplies.
They are at capacity (or over capacity), meaning not only will COVID-19 patients eventually be turned away, but patients in need of non-COVID-related medical care will too.
Patients like my child.
Or your child.
Or you, your spouse, your parents, or your siblings.
It’s already happening, and one tragic case from Madrid should be the eye-opening story that hopefully wakes stubborn Americans up to this reality.
As reported in The New York Times, last March, as COVID tore across Spain and other European nations, a nursing home worker named Lídia Bayona Gómez began vomiting and coughing. She self-isolated and got tested for COVID, but the results came back negative—twice. However, her weight continued to drop, her urine turned red, and Lídia got sicker. By April, after repeated attempts to see a doctor, she had a phone consultation through which she was prescribed medicine for gastroenteritis and a urinary tract infection and was told to stay home.
The treatment didn’t work, and her pain worsened. “In late June, her sister took her to an emergency hospital unit,” The New York Times article shares. “In mid-July, she underwent a 12-hour surgery to remove two cancerous tumors, one from an ovary and the other from the bile ducts. She died in the hospital nine days later, at age 53.”
Lídia’s case is not an isolated one. The article also references the case of another woman who has learned she has terminal cancer after trying for seven months to get into a hospital for testing. And another, a woman named Sonia, who died at age 48 from colon cancer after after failing for three months to see a doctor in person.
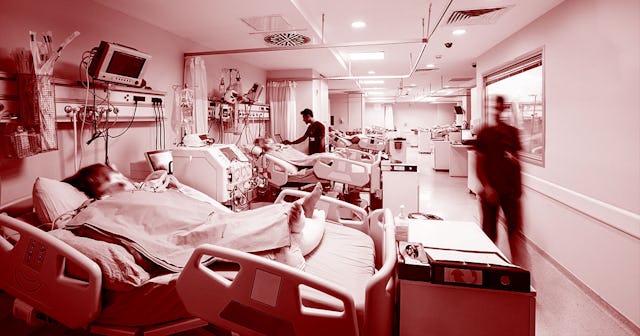
Jackyenjoyphotography/Getty
“Hospitals and other health care centers have been forced to devote most of their resources to COVID-19 patients, and doctors are warning that a growing number of cases of cancer and other serious illnesses are going undetected, which could end up costing many more lives,” The New York Times goes on to say.
This rippling effect—the inability to access medical care we need—will be felt, if it’s not already, across America. We need to brace for the terrifying reality that we might need to see a doctor, that we might need a hospital bed, and we might be told there’s no room for us.
Doctors, nurses, and medical staff are overwhelmed and are forced to prioritize COVID-19 patients as the world tries desperately to get this pandemic under control. There are only so many of them. There are only so many beds. There are only so many rounds of medication and IVs and bags of blood. It’s hard to fathom in a modernized nation in 2020 that any of that could run out.
But it can. And it will if things don’t change drastically.
Just look at Houston, Texas, where in July hospitals across the city were full, forcing ER patients to wait for hours to be treated, and where ambulances were being diverted to other hospitals, but then those hospitals were at capacity, leaving patients with nowhere to go. Hospital officials were eventually able to add beds and increase staff, but that’s not something that can be done overnight, explains The Texas Tribune.
“Those things are not like a switch-key type of activity,” said Harris Health System president and CEO Esmaeil Porsa. “As you can imagine, ICU nurses are not a dime a dozen. They are very hard to come by, and it takes time to actually be able to do that.”
Porsa also describes that normally, an ER patient is evaluated and admitted into a bed quickly, but this summer in Houston hospitals, there were no beds—not even for some COVID patients who should not only be in a bed, but also need to be isolated. “Normally that patient would just go to an ICU bed, but because there are no beds available, they continue to board in the emergency room. This is not something we would choose to do. The only reason this is happening is because we are being forced to do it.”
And now that we’re well into the fall and seeing newer, more intense COVID surges, states that this summer may have had calmer hospitals with plenty of available beds are now seeing the terrifying reality that Houston experienced this summer.
Utah, for example, is one such state. NPR reports that Utah state health officials have already warned that “hospitals may soon be forced to ration care because of limited ICU space.”
And if you don’t know what that could mean—”rationing care”—listen to the tragic story of NYC resident Luis Arellano, who, in the spring, went to three different hospitals when he showed COVID-19 symptoms. He was turned away at one, told to come back if he got worse. At another, he was told he’d have to wait seven to nine hours to be seen because he wasn’t sick enough yet. However, by the time he finally was deemed sick enough to warrant a bed, it was too late. COVID had ravaged his body and he died on April 5.
And in rural Wisconsin, which is seeing a huge surge in cases right now, the same is happening. The Marshfield Clinic Health System, which runs nine hospitals in primarily rural parts of the state, is expecting the number of COVID-19 patients to double, if not more, by the end of the month, NPR reports. And again, the problem isn’t just beds—it’s medical staff to take care of the sick people in those beds. Specialized medical staff that can be hard to come by. “That will push us well beyond our staffing levels,” says Dr. William Melms, chief medical officer at Marshfield. “We can always make more space, but creating the manpower to take care of our patients is the dilemma.”
In states like Utah and Wisconsin, the fates of Luis Arellano and Lídia Bayona Gómez could be repeated as hospitals become more and more full, and as staff is stretched thinner and thinner. COVID and non-COVID patients could be forced to wait hours, days even, for medical care, or turned away altogether if numbers continue to surge from state to state.
Also, it’s important to note that back in the spring when hospitals in the Northeast were overflowing with COVID patients, and Luis Arellano was struggling to find a one to admit him, those states were on lockdown so other types of ER-related issues were at a minimum. In Houston this summer, the state was open, meaning ERs were still seeing “a steady flow of patients in need of care as a result of car accidents, violent crime and heat-related medical emergencies,” says The Texas Tribune.
So, as we continue to see an uptick in cases nationwide, it’s imperative more than ever, with medical staff hitting the 9th month of exhausting round-the-clock shifts, depleted supplies, and mental and physical fatigue we cannot imagine, that cities and states implement new lock-down measures. We need to reduce the number of injuries and illnesses caused by people being out and about so that doctors and nurses have space, time, supplies, and beds to adequately manage the patients in need of critical care.
Hospitals around the nation continue to scramble to meet the needs of all patients—COVID and non-COVID, but expanding, making more room, and hiring more staff takes time. They need us to do our part as they do theirs. The need us to stay home, wear masks, wash our hands, and practice social distancing as they work frantically to prepare for more sick patients. They need us to do everything we can to stay healthy, keep our loved ones healthy, and stop the spread.
“I simply cannot give a patient adequate attention when I have recently had to see 100 people in a single day,” Dr. Patricia Estevan, a Madrid public health care doctor, confesses.
Medical professionals are doing their best, but if our country continues to ignore their pleas, not even their best will be good enough to save us.
This article was originally published on