My Healthy Teen Wound Up In The ICU With COVID-19
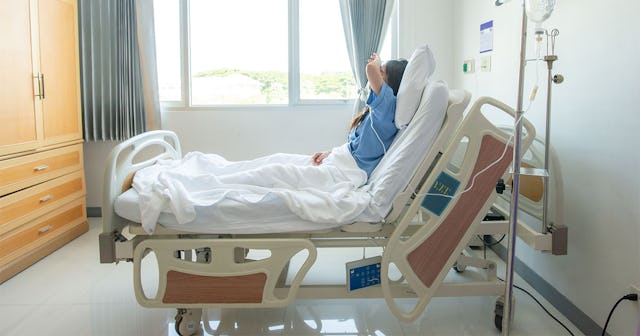
Beep, beep, ring, the alarms were going off … red light, blue light. I jumped off the makeshift bed I made in the corner of a small chair to check on my son. I quickly glanced at the monitors that displayed his vitals on my way to his bed. Finally reaching his bed, I was able to see and feel with my hands the shallow rise and fall of his chest. I knew this would result in a slew of nurses entering his room in minutes. They had cameras all over the room to keep watch on him 24/7. It would be a few minutes for them to dress in personal protective equipment (PPE).
This is COVID-19.
My son is a very healthy, active 16-year-old. He has no underlying health problems; the only time he has been to the hospital was for a broken arm due to a wipeout while snowboarding a difficult trail. Statistically, this should have never happened. Months of reports claimed that healthy children were safe. Parents were complaining that kids shouldn’t be doing virtual school because they would be safe and wouldn’t have dire effects of COVID-19.
I think I should rewind and explain how he ended up in the ICU in one of the top children’s hospitals in the country. I will begin back when we first heard of COVID-19. Everybody dealt with the news of a new deadly virus invading our lives differently. Our family took it seriously and decided to do everything possible to avoid getting it. We stopped going to stores and ordered in all of our groceries. Once they were delivered, we would quarantine them in a separate fridge for three days. The entire family worked from home. We quarantined our mail for three days.
When there was a mask mandate, we opened our lives up a bit more and started to venture to the local grocery stores, armed with multilayer masks, gloves and hand sanitizer. Time spent with friends and family was now via zoom and FaceTime gatherings. As life tends to, it must keep turning. This resulted in having to go back to the office to work. Fall came and school opened back up. Exposure to the outside world also meant possible exposure to somebody who had COVID-19.
Although we will never know exactly how the deadly virus came into our house, we do have recollection of a store with an anti-masker coughing. Or maybe it was the person at the office who we later found out was asymptomatic but had a family member who was diagnosed. It started with my daughter coming home one day feeling under the weather. It quickly turned to her feeling extremely sick; sore muscles, burning nose, headache, upset stomach, cough, fever, loss of taste/smell and difficulty breathing. Having heard the symptoms, we decided to get her tested immediately. She would soon find out she was positive.
While awaiting the result, she quarantined herself from the family using her bathroom and staying in her bedroom. The next day, I started feeling sick with similar symptoms. The body aches were the worst that I have ever felt in my life. This was followed by high temperature and difficulty breathing. I dug out our pulse oximeter and monitored the readings. Luckily, both my daughter and I hovered around 90.
Mansoreh Motamedi/Getty
My husband moved out of our bedroom and into the basement family room. My nine-year-old daughter woke up the next day with a nose burn and a slight headache, but was feeling better the following day. Feeling we had done a good job of containing the virus, we survived as a family isolated in our separate rooms and stayed in contact by communicating via text and the House Party app.
That weekend, my husband and son raked the leaves from our acre of land as I watched them from my bedroom window, longing to join them. My youngest daughter and oldest daughter (we have three daughters) played outside in the leaves. I was looking forward to counting down the days until I was done isolating in my room and could join my family and give them huge hugs. Little did we know this was only the beginning of our COVID journey.
The next day, my husband and son mentioned that their bodies were sore. I hoped it was from an afternoon of raking leaves. Over the next few days, they developed a cough followed by similar symptoms that my daughter and I experienced. My 10 days of quarantine ended, and I was able to see my family in person. My son was quarantined upstairs in his room, while my husband quarantined in the basement family room. Since we already had COVID, my middle daughter and I were able to see them and keep them company.
At first, they seemed to have very similar cases to what we experienced, but this quickly changed. My son’s fever spiked to 105.7. I immediately called the doctor to verify the hospital’s COVID precautions, then rushed him to the Emergency Room. He was given chest X-rays and found to have bilateral pneumonia. They administered an IV and medication to get his fever under control. After a day in the ER, they sent us home that night with steroids and an inhaler to help him breathe and instructions to bring him back if his oxygen level dropped.
That evening, his temp began to rise again. His breathing was difficult, but the inhaler helped for a while. The next day was tough for both my son and husband. My husband was developing an equally super high temp and his breathing was getting more and more difficult. Per the doctor, we treated it with Tylenol and kept an eye on his oxygen level. It hovered around 89.
It was very strange seeing my husband, who hasn’t been to the hospital the entire two decades we have been married, down and out. This is the man who has no underlying health conditions, runs half marathons, backpack camps off the grid in the most difficult trails and conditions every year with my son for a week. They travel to Canada and hike for 60+ miles, carrying all of their supplies for a week on their backs.
As the day progressed, so did the symptoms of my son. His fever was spiking once again and his breathing was becoming increasingly difficult. In a very short period of time, his pulse ox dipped to the low 80s and was rapidly declining. I immediately told him we were headed back to the hospital. He was so weak; it was difficult getting him down the stairs and into the vehicle. As I rushed out the door, I told my middle daughter to monitor her father and check his temp and oxygen level every 15 minutes.
When we arrived and checked into the hospital, my son had soaked through his clothing with sweat and was having an extremely difficult time breathing. They took his pulse oximeter level and it was down to 74. They immediately hooked him up to an oxygen mask and had to keep increasing the level of flow. They took more X-rays and gave him more medicine to lower his temperature, which now was a scary 106.
rubberball/Getty
While waiting for the labs to come back from his blood draws and X-rays, my phone rang, and it was my daughter. She informed me that my husband’s condition was declining, and he was being brought into the hospital. I sat in the chair next to my son’s bed, watching him struggle for breath, while awaiting my husband’s arrival. Fear ran through my veins.
Although it seemed like hours, it was shortly thereafter that they wheeled my husband into the room across from my sons’ room. They hooked him up to oxygen, took chest X-rays, drew blood and started medicine. I was only allowed in the ER because my son was underage and I had already had COVID-19; otherwise I would not have been allowed to be there. The hospital staff was amazing and relayed what was happening in my husband’s room. They understood how incredibly hard this was.
The doctor informed me that my son’s condition was very serious and they would have to transfer him. He was far too serious to be transferred to the closest children’s hospital and would have to go to one of the country’s top children’s hospitals. As we waited for the transport ambulance, I was informed that my husband would be admitted to the hospital. They let us wave goodbye to my husband as they wheeled him out of the ER and to the elevator to take him upstairs to the COVID unit. A short time later, the ambulance came to transport my son to the children’s hospital. Again, because he is underage and in serious condition, I was able to accompany him.
The ambulance ride was a blur; holding my son’s hand while watching the EMT change the oxygen tank because he had already gone through the first one. Finally, we arrived.
This brings me back to the beginning of my story. With many medical doctors, infectious disease experts, medical tests, powerful medications and lots of oxygen, my son got better. He eventually was transferred out of ICU and into acute care. Over time, he graduated from his oxygen mask and was able to have a nasal tube and finally no oxygen. He had terrible rashes from the meds administered to him multiple times a day and really didn’t like the twice daily shot into his stomach. He is extremely strong and handled it like a champ.
While I was at the children’s hospital, my husband was at the local hospital 100 miles away isolated in the COVID unit. Thankfully, we could text and FaceTime, even though some days he didn’t have the energy or breathing ability to last more than a few minutes. My son was released from the hospital and two days later my husband was also released, joining us at home.
It was a long journey fighting COVID-19, but it made our already strong family stronger. Time has passed, but we still feel the effects of COVID-19. My husband and son’s lungs still aren’t at full capacity and at times physical activity leaves them exhausted. My daughter and I are still experiencing lack of smell, some taste loss, and substantial hair loss. Most reports don’t inform you of long-lasting symptoms, but they are very real.
COVID can affect even extremely healthy people and bring them to their knees. In our family of six, two people were hospitalized, two people had a very bad case, one had a day of a slight cold and one was totally asymptomatic. Proof that nobody can predict how this powerful virus will attack your body. Although wearing a mask vs. not wearing a mask has been made into a political statement by some, it absolutely shouldn’t be.
I know this will bring about the discussion from a few wondering, do masks really protect since you were wearing one and caught COVID-19? Studies have shown that for full possible protection both people must be properly wearing their masks. If one person is wearing a mask and the other isn’t, there is a medium risk of exposure. In comparison, if both people are properly wearing their masks, the risk is now reduced to low risk of exposure. Add to that 6 feet of social distancing and the number decreases again.
Please wear your mask to protect you, your loved ones, and innocent strangers. All it takes is one careless person.