The HPV Vaccine Could Eliminate Cervical Cancer Entirely, New Study Finds
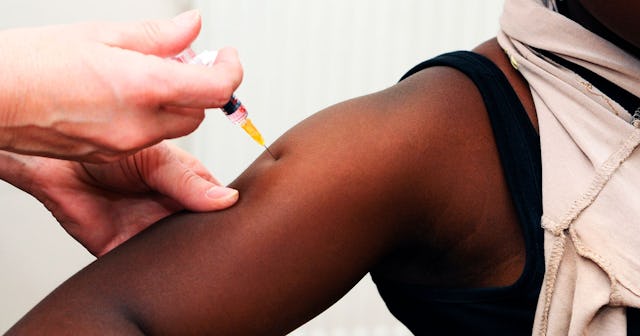
New study confirms the vaccine ‘exceeds expectations’ with benefits
A new study finds that the HPV vaccine is far more effective than initially expected. The vaccine, which was first introduced back in 2006, has been implemented in more than 115 countries and territories. The study shows that the benefits of the vaccine extend beyond those who receive it, which is huge. HPV is the leading cause of cervical cancer, and the vaccine could eventually lead to the elimination of cervical cancer altogether.
Currently, the World Health Organization recommends girls ages nine to 13 receive two doses of the vaccine, Gardasil, which protects against nine strains of HPV. HPV, or human papillomavirus, is the leading cause of cervical cancer. The virus can also cause other cancers, including cancers of the penis, head and neck, as well as genital warts.
The new study suggests that the more people who receive the vaccine, the better for everyone overall. The vaccine not only reduces HPV infection rates and the presence of precancerous cells in the cervix in people who receive the vaccine, but it also reduces rates of HPV-related diseases in people who have not been vaccinated.
A U.S. federal advisory panel now recommends that the HPV vaccine be given to both men and women up to age 26, based on the study’s findings.
One of the more noteworthy findings is that the HPV vaccine led to a reduction in abnormal Pap smears. Pap smears are used to detect abnormal cells found in the cervix, which can sometimes develop into precancerous cells or cancer. The researchers in the study found that, five to nine years after receiving the vaccine, a reduction of more than 50 percent in cases of pre-cancerous cells was apparent in girls age 15 to 19.
“The impact of the HPV vaccination has actually exceeded expectations,” Lauri Markowitz, associate director of science for HPV at the Centers for Disease Control and Prevention, who worked on the study, tells NBC News. “The trials showed that HPV vaccines are very effective, and data from the real world has confirmed that.”
As for herd immunity, well, this vaccine is the bee’s knees. In countries where at least half the population received the vaccine, researchers saw evidence of herd immunity — a decrease in the prevalence of HPV-related diseases was apparent even among those who were not vaccinated. This is because vaccination leads to fewer HPV hosts — herd immunity, folks. It’s REAL.
Unfortunately, despite all of this scientific evidence and the major benefits to the HPV vaccine, the rate of vaccination against it in the U.S. is lagging behind other countries. While the U.S. was the first country to make the vaccine available to all genders, the CDC finds many parents and health care providers aren’t really vaccinating boys. Even though there are often no detectable HPV symptoms in males, who then unknowingly spread it to their sexual partners.
Sigh.
Despite the impressive findings, Pap smears and HPV screenings are still vital to the community when it comes to reducing (and possibly eliminating) cases of cervical cancer.
“Vaccination and screening together make a program,” Diane Harper, senior associate director of the Michigan Institute for Clinical Health Research, tells NBC News. “Very few HPV cases progress into cancer, but the only way we’re going to find those that do is through the screening program.”