Mom Shares Tragic Story Of Breastfed Infant Dying From Starvation
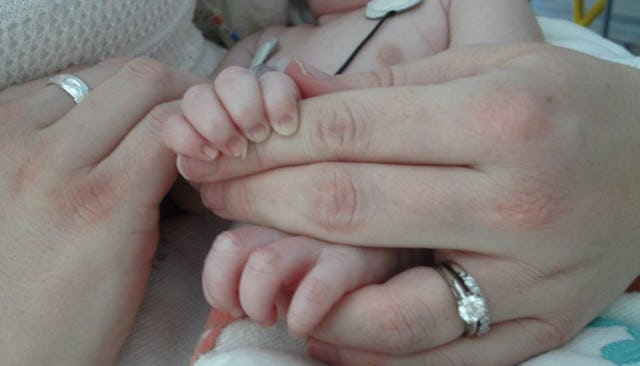
Doctors and nurses told her to keep nursing, despite signs that her son wasn’t thriving
Five years after losing her infant son, a mom is sharing the heartbreaking story of his life and death in the hopes of helping other parents. Her baby died of starvation, as the new mom was encouraged to keep nursing despite warning signs that he wasn’t getting enough breast milk. Her story is an important one that every expecting mom who plans to breastfeed should read.
In a blog post for The Fed Is Best Foundation, Jillian Johnson writes of her heartbreak as the five-year mark of losing son Landon approaches. It’s taken this long to work through her pain and also the fear of what others might think. “I wanted to share for a long time about what happened to Landon, but I always feared what others would say and how I’d be judged. But I want people to know how much deeper the pain gets.”
Johnson was like so many moms who plan to exclusively breastfeed their babies. She delivered Landon in a baby-friendly hospital, which is a hospital geared toward encouraging moms to nurse their children. As she explains, “Unless you’d had a breast augmentation or cancer or some serious medical reason as to why you couldn’t breastfeed, your baby would not be given formula unless a prescription was written by the pediatrician.”
Landon was born full-term via emergency c-section with a healthy birth weight and strong Apgar scores. A few hours after the surgery, he was on Johnson’s breast with “an excellent latch” for 15-40 minutes every 1-2 hours.
“Landon was on my breast – ALL OF THE TIME. The lactation consultants would come in and see that ‘he had a great latch and was doing fine’ but there was one who mentioned I may have a problem producing milk.” That problem was PCOS (polycystic ovarian syndrome), a hormonal condition that can make it harder for affected women to produce milk.
Despite knowing this risk factor was present along with several others, as explained by physician R. Christie Del Castillo-Hegyi who assisted Johnson in writing her blog post, the new mom was encouraged by nurses, lactation consultants and doctors to keep nursing. It became quickly apparent to Johnson that something was off.
“Landon cried. And cried. All the time. He cried unless he was on the breast and I began to nurse him continuously. The nurses would come in and swaddle him in warm blankets to help get him to sleep. And when I asked them why he was always on my breast, I was told it was because he was ‘cluster feeding.'”
Johnson remembered hearing about cluster feeding in the parenting classes she took before her son was born. That knowledge, coupled with the medical personnel telling her that Landon was doing well, kept her going with nursing, despite her son not gaining any weight. In fact, he was losing it.
Dr. Castillo-Hegyi writes, “By the first 24 hours, he had nursed a total of 9.3 hours, had zero wet diapers and four dirty diapers. By 27 hours, he had lost 4.76%. His nursing sessions became longer and longer until he was on the breast continuously by the second day of life. On the second day, he produced 3 wet diapers and 6 dirty diapers and nursed for almost 14 hours total. By 53 hours of life, he had lost 9.72%.”
Despite all of the hours he spent nursing, Landon was never satisfied. A sign that Johnson realizes now wasn’t good. “Did you know newborns aren’t supposed to cry all the time? They’re supposed to eat and sleep and dirty their diapers. I had no idea that he was inconsolable because he was starving – literally.” Dr. Castillo-Hegyi explains, “If a mother’s colostrum does not meet the child’s caloric requirement, they will breastfeed for hours a day in an attempt to relieve their hunger. A child who is ‘cluster-feeding’ may actually burn more calories breastfeeding than they receive in return, which can result in fasting conditions and accelerated weight loss.”
Landon was discharged after losing 9.72% of his bodyweight and, 12 hours after coming home, went into cardiac arrest as a result of dehydration. After his parents discovered him unresponsive, pulseless and blue after falling asleep cluster feeding, they called 911. He was rushed to the hospital, where after much intervention, he regained a pulse. He was then placed on life support, where he spent 15 days before passing away after it was decided that his prognosis was too poor to keep him on it.
Johnson writes, “I still have many, many days of guilt and questions – what if I would’ve just given him a bottle? And anger because how would I have known,” she continues. “And the best advice I was given by one of his NICU doctors while he was on life support is sure breast is best, but follow with the bottle. This way you know your baby has eaten enough…if only I could go back in time.”
Of course, what happened to baby Landon was rare, as many babies lose weight in the first days of life before a mother’s milk fully comes in. But if his story can save just one baby from a similar fate, his parents feel it was worth sharing. They encourage parents to check out The Fed Is Best Foundation’s weighing protocol and feeding plan for helpful information about infant feeding.
Johnson is taking what positives she can from such a tragic outcome. “That little boy gave me ten of the most incredibly life changing months. I’ve been humbled. Challenged. My relationships have fallen apart. Some have come back together. I’ve learned forgiveness. And the true meaning of ‘life is short.’ I love hard – to a fault. But I couldn’t live with myself knowing his death was in vain. I’ve learned so many lessons. I’ve learned the true meaning of compassion and unconditional love.”
This article was originally published on