A Blood Clot Almost Killed Me After My Pregnancy. Here's What You Should Know.
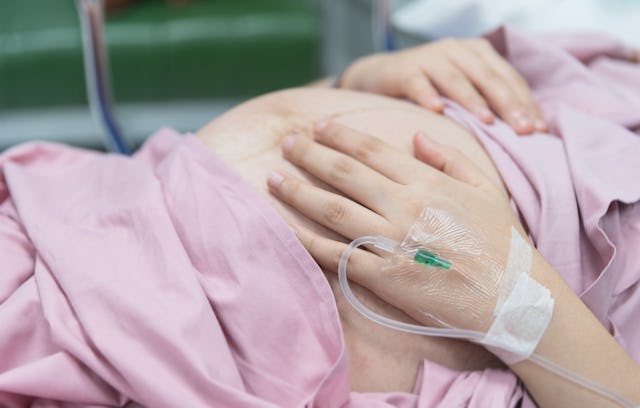
When I was twenty-two, I was diagnosed with Factor V Leiden, a genetic clotting disorder that causes blood to clot more than normal. I was diagnosed with the condition after I developed a massive deep vein thrombosis (DVT) in my left leg.
Because I was a healthy, active 22-year-old, no one could understand why I would develop such a massive clot. I didn’t have any known risk factors, so my doctor ordered tests, which uncovered the clotting mutation.
When my medical team explained the condition to me, they told me many women don’t discover they have Factor V Leiden until they try to start families and experience unexplained miscarriages—particularly late-term losses. I was told I would need to resume blood thinning medication if and when I ever became pregnant to counter the effects of the Factor V mutation and to reduce my risk for developing another DVT.
When I received my diagnosis, I was years away from having kids, so for a long time, the information sat idly in the back of my brain. I won’t lie—I worried. I wondered if my clotting disorder would cause complications for me or pose a danger to my future children.
Two years after my DVT, I learned that I also had something called “May Thurner Syndrome,” a condition where my iliac vein was compressed by an overlying artery. This too was determined to be a contributor to my initial DVT and to the post-thrombotic syndrome I experienced in the years afterward.
So, at twenty-four, I underwent a vascular procedure to open the iliac vein with a mesh stent.
When I was twenty-nine, I became pregnant with my first child. I started taking Lovenox, an anticoagulant administered by syringe, within days of learning I was pregnant per doctor recommendation.
At 36 weeks, I was switched to Heparin, an anticoagulant that remains in the blood stream for a shorter time than Lovenox does—an important change in preparation for childbirth since I could bleed out otherwise. I was monitored closely by my doctors and ultimately did not have any complications during pregnancy or postpartum.
Three years later, I became pregnant with twins. Again, I started Lovenox early in my pregnancy, switched to Heparin in late pregnancy, and resumed Lovenox until I was six weeks postpartum per doctor recommendation.
It was easy to be lulled into a false sense of security. Many years had passed without further clotting incidents. I had met other women with the same condition who had successful pregnancies—some without taking medication.
Nevertheless, I worried a lot during my pregnancies, especially knowing that many Factor V losses occur in later pregnancy. Although I never personally experienced these problems, I never fully felt safe or at ease. I always worried that my condition would sneak up on me when I least expected it.
However, that worry would dissipate as soon as I delivered. Though I was still statistically at risk for clotting during the first six weeks after childbirth, I felt I was out of the danger zone when my kids were born. More than anything, I was relieved they arrived unscathed despite my increased clotting risk.
After pregnancy, I took my medication as prescribed, but with much less enthusiasm. With my babies on the outside, the instinct to protect them was no longer the driving force as I injected myself with a syringe full of anticoagulant every night.
When I stopped the Lovenox exactly six weeks after the birth of my twins, I wanted to celebrate. I was out of the woods. I resumed the daily aspirin I took preventatively in my regular life.
Having finally healed from an arduous twin pregnancy and C-section, I started taking my older son to activities again. I took the kids on walks. I resumed spinning, running, and resistance training.
I felt good. Slow, and kind of like I had been hit by a freight train—a freight train named 15 lbs. of baby—but good.
Then, at 9 weeks postpartum, I noticed a tightness around my right quadricep. I assumed it was a sore muscle. I jogged extra slowly on it. I stretched and foam rolled (I cringe so hard now thinking about how dangerous this actually was). I continued my normal activity until a few days later when I realized my symptoms could be something more.
I noticed that I could suddenly “sense” my right leg. It seemed slightly larger—not yet enough that it was obvious, but enough for me to notice. I also noticed that the tightness wasn’t going away. I was suspicious. I had seen this show before, and I knew how it ended.
I called my doctor right away and asked for a same-day ultrasound for a suspected DVT. I explained my history and symptoms and was scheduled for an appointment that afternoon.
In the hours that followed, my symptoms worsened exponentially. My leg nearly tripled in size. The color changed. Pain increased. By this point, I knew what I had. I was just waiting for my official diagnosis. That evening I received it—a massive DVT that ran almost the full length of my right leg. By that time, I could barely walk.
You might wonder how I didn’t know it was a DVT right away since I had one before. There are several reasons why.
First, I had experienced many “false alarms” in my life following my initial blood clot. There were times in the years after my diagnosis that I’d immediately go to the hospital or doctor for a new pain in my leg, worried it was another DVT, only to find it was tendonitis or some other benign issue.
Second, I was recovering from a physically difficult twin pregnancy and C-section. Aches and pains were a part of daily life. Ibuprofen and I were on a first name basis.
Third, I was just getting back into working out after taking nearly ten months off because of my twin pregnancy and C-section. Again, some muscle soreness was par for the course, and my initial DVT symptoms were difficult to discern from this. This was true of my first blood clot as well. As a runner and weightlifter, it was initially hard to tell the pain apart from muscle soreness.
Fourth, I was nine-and-a-half weeks postpartum. Statistically, I was out of the woods. Blood clot was not my first thought.
It wasn’t until a few days after my symptoms arose, when I noticed my self-care and monitoring weren’t helping, that I suspected the problem was something bigger.
Hindsight is 20/20, but if you take anything away from my experience, let it be this:
1. Know your own risk of developing a DVT.
Consult your doctor. DVTs on their own are painful and physically damaging to the affected limb, but the real danger, the thing that could literally kill you, is the fact that the blood clot can break loose, travel through your bloodstream, and cause a pulmonary embolism (PE).
2. Don’t take your condition for granted.
If you have a clotting disorder, or if you are at increased risk for developing a DVT for other reasons, don’t take your condition for granted. I don’t mean to scare you. I hated hearing bad stories involving Factor V Leiden during my pregnancy—so much so that I didn’t even read them—but you should at the very least be aware of your condition and individual risk.
3. Don’t take less protective care of yourself after pregnancy.
Motherhood has this way of removing us from the center of our own universe. Whereas caring for ourselves is our driving force before kids, after kids, it’s easy not to focus on our health even when it matters most.
If you took Lovenox or Heparin during pregnancy and are prescribed to take it through six weeks postpartum, it may be tempting to skip an injection or two once it’s just you occupying your body once more. Don’t skip it. Take care of yourself like your life depends on it—because it just might.
4. Monitor, monitor, monitor.
Twice in my life I’ve had a major DVT and each time I did not know right away. Thankfully, my second time, I knew the signs to look for. The pain that doesn’t dissipate. The increased swelling and change of color in the limb.
If you don’t know the signs, Google them. Right now. Literally go and Google “signs of DVT.” If you have even the slightest worry that you might have one, call your doctor and tell them you want a same-day ultrasound for a suspected DVT. If that’s not an option, go to a hospital ER or urgent care center. The sooner you can be evaluated, the sooner you can catch the problem and start taking medicine and reduce your risk of the clot worsening.
5. If it happens to you, don’t lose heart.
Receiving my second DVT diagnosis at nine weeks postpartum was a pretty big physical and psychological blow. I mean, here I was, just getting back into a groove with fitness and the kids, and BAM—huge physical setback. I not only felt like I was back at day one after my C-section, impairment-wise; I felt like I was back at day one of the first time I was diagnosed with a DVT eleven years earlier. Even when you’re expecting it, the reality of the diagnosis is still a shock.
So, if you’re diagnosed with a blood clot during pregnancy, postpartum, or any time in your life, know that others understand. I know how much it sucks. I know that recovery doesn’t just take days. I know it can take weeks, months, and years. I know that for some, it will be a lifelong problem. I will be on daily anticoagulant medication for the rest of my life, pregnant or not. That’s pretty heavy stuff. But know that this too shall pass. Remember that you are a tough cookie and that you will emerge stronger. You got this, mama.