An Open Letter To Blue Shield Of California HealthCare
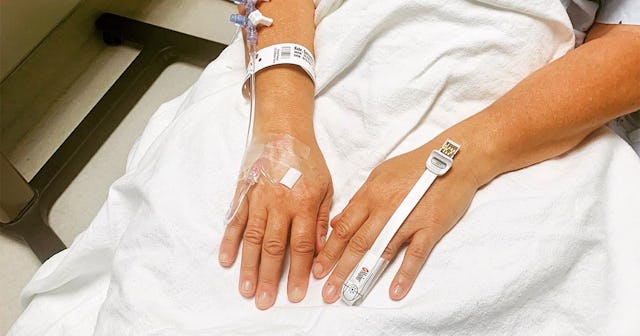
I’m quite sure I’m not the Blue Shield of California “member of the month.” Since I was diagnosed with breast cancer at a young age, my surgeries, medications, tests and doctor visits must have reached millions of dollars.
In the US, we’re extremely lucky to have access to some of the best health care in the world. As a breast cancer survivor, I count on the latest technology, testing, and research, and rely on the ability to choose (with my medical team) what will keep me alive to see my boys graduate. Unfortunately, the health care industry is a billion dollar business that seems to be more concerned with profits and annual revenue than providing affordable and easily accessible treatment for their members.
I have a top tier Blue Shield of California PPO plan at a significant monthly cost, and still have to pay out of pocket for many tests and medications each month, on top of my (expensive) monthly payment.
Courtesy of Sam Kuhr
What I don’t expect is to fight Blue Shield of California for coverage that they are legally obligated to provide.
According to the American Cancer Society, “The Women’s Health and Cancer Rights Act (WHCRA) helps protect many women with breast cancer who choose to have their breasts rebuilt (reconstructed) after a mastectomy. Mastectomy is surgery to remove all or part of the breast. This federal law requires most group insurance plans that cover mastectomies to also cover breast reconstruction. It was signed into law on October 21, 1998. The United States Departments of Labor and Health and Human Services oversee this law.”
I was recently scheduled for a revision to my double mastectomy, and two days before this scheduled surgery (on February 4th, International World Cancer Day), I was notified that Blue Shield of California denied this surgery. Obviously there was much anxiety and stress preparing for this significant surgery, and this denial felt more upsetting since it seemed to be in direct violation of The Women’s Health and Cancer Rights Act.
Ashkan Forouzani/Unsplash
I had two choices: reschedule this surgery and let my doctor’s office handle it or fight this denial. I had not only been mentally preparing for this surgery, but Hot Hubby and I had spent weeks logistically preparing as well. So I decided to fight.
I was mad. I was mad I had cancer in the first place. I was mad I had to have a double mastectomy to remove my womanhood. I was mad I had to have a revision to correct this surgery. I was mad this would be my 10th surgery/procedure in five years. I was mad my boys were again worried that mom was going in for surgery. But I was mostly mad that my healthcare company, to whom I pay a shit ton of money each month to protect my health, was rejecting me. I felt completely abandoned. I was also mad for other women, who perhaps might not be aware of their healthcare rights, and have received a similar letter denying them coverage for something they are entitled to under federal law.
I had exactly 24 hours before my surgery was scheduled, and I decided I was all-in to fight for this denial to be overturned. I realized the normal appeals channel would not work for me in my time frame; I needed a radical approach. I was able to track down the name of every member of the Blue Shield of California leadership team (the internet is a wonderful thing!), figured out their email configurations, and sent each member of the executive team a letter.
Almost immediately, I received personal responses from five Blue Shield of California executives expressing concern and offering to “pass this along to the correct channels” to help resolve the issue. I had their attention.
Matthew Henry/Burst
For the next six hours, I worked relentlessly via email with Matt B., the extremely helpful and knowledgeable patient liaison who worked with me, the Blue Shield doctor (who denied the surgery without knowing me, my body, my medical history or the reason this surgery was medically necessary) and my personal doctor (who knows my body intimately and has seen it from the inside many times). A peer-to-peer call was facilitated to discuss my case and why it was medically necessary.
Finally my surgery was approved — 14 hours before I was scheduled to check in at the hospital.
I needed to quickly shift gears to prepare my mind and body for yet another invasive surgery, and mentally regroup.
But I couldn’t shake this. I was still mad. I was mad that this was so difficult. I was mad for other breast cancer survivors who have had their revision surgery denied, and perhaps just accepted this as another horrible part of cancer. I was mad for the women who wouldn’t even have the first idea that they could even fight this. I was mad for women who didn’t have the time or luxury to dedicate a whole entire day to fighting for their rights.
I sent another email to each member of the Blue Shield of California leadership team who responded to me.
A few of their executives sent a cursory reply thanking me for bringing it to their attention, et cetera. However, here are nine things I’d like Blue Shield of California to know:
Courtesy of Sam Kuhr
1. My breast cancer was not elective. In fact, when I was diagnosed, it was the worst day of my life.
2. I should not have to fight for procedures and treatments that are medically necessary for my survival.
3. I am protected by a federal law, and should not have to quote the law to my healthcare provider in order to get my coverage approved.
4. I worry for other women who may not have the energy or know-how to fight for their rights in a “David and Goliath” situation.
5. It turns out that some color photos were all that was needed to get this surgery approved immediately; instead of sending out a straight denial letter prompting immediate anxiety, perhaps consider sending out a “pending further information” letter. It seems a little more humane.
6. Matt B., the gentleman who helped me navigate this under the clock, was incredible and showed me care and empathy when I needed it. You should give him a raise. We need more people like Matt B. being the face of healthcare, instead of an impersonal denial letter.
7. I appreciate you correcting this “oversight” — however, at the risk of sounding cynical, you do stand to save a few hundred thousand dollars for each surgery you deny. I am wondering out loud here, so bear with me … could it be you are actually hoping people don’t fight these denials to get the coverage they are entitled to? It sure would save you a ton of money.
Courtesy of Sam Kuhr
8. Please learn from this example of how the system failed and make changes to provide healthcare and communication that is worthy of your friends and family.
9. I will be needing testing and procedures for the rest of my life. That’s how it looks for me now as a cancer survivor. Please don’t make me fight for my coverage again. I’m tired, and each procedure takes it out of me mentally and physically.
Hopefully you are never in the position to have to fight for your healthcare. However, if you’re unsatisfied with the response from your insurance company, or you have an urgent health problem, you should contact the agency charged with regulating your plan. If you live in California, these agencies are the DMHC or the CDI. For those outside of California, the easiest way to find out which agency oversees your plan is to call the consumer hotline number for either agency and ask a representative. The consumer hotline for DMHC is (888) 466 2219. For CDI it’s (800) 927-4357.
Blue Shield of California had the following comment: “We cannot comment on any member case due to federal privacy laws. However, we do take access to care for our members very seriously and will always work with them to help ensure they receive the care that they need.”
For additional information:
https://www.dol.gov/general/topic/health-plans/womens
https://healthcare.findlaw.com/patient-rights/womens-health-and-cancer-rights-act-overview.html
This article was originally published on