Don't Let Your 'Delayed Cord Clamping' Turn Into A 'Lotus Birth'
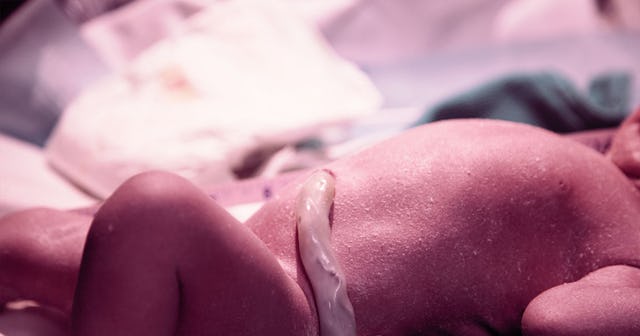
As an anesthesiologist, I recently took care of a patient who needed an emergent C-Section, and she requested that the umbilical cord not be cut “until it was white.”
I’ll be honest, I had no idea what she was talking about.
A bit of googling later in the day, lead me to believe what she was referring to was the process of delayed cord clamping (DCC).
What is delayed cord clamping?
Before the mid 1950s, the term early clamping was defined as umbilical cord clamping within 1 minute of birth, and late clamping was defined as umbilical cord clamping more than 5 minutes after birth. In a series of small studies of blood volume changes after birth (primarily conducted in the late 1960s) , it was reported that 80–100 mL of blood transfers from the placenta to the newborn in the first 3 minutes after birth, and up to 90% of that blood volume transfer was achieved within the first few breaths in healthy term infants.
However, a lack of specific recommendations regarding the practice actually lead to continued shortening of the time interval from birth to clamping of the umbilical cord, with common practice being in as few as 15 to 20 seconds.
Subsequent, well conducted studies, including randomized controlled trials of term and preterm infants as well as additional physiologic studies have evaluated the effects of immediate versus delayed umbilical cord clamping. Importantly, delayed cord clamping is usually defined as 30–60 seconds after birth.
RyanJLane/Getty
Indeed, delayed cord clamping does seem to have some benefit: In term infants, delayed umbilical cord clamping increases hemoglobin levels at birth and improves iron stores in the first several months of life, which may have a favorable effect on developmental outcomes. In preterm infants, rates of intraventricular hemorrhage (a type of bleeding in the brain that can occur in preterm infants) and necrotizing enterocolitis (a devastating infection of the intestines) are lower, and fewer newborns require transfusion when delayed umbilical cord clamping is employed.
Given this, several major health organizations now advocate for delayed cord clamping, including the World Health Organization, the American Academy of Pediatrics, and The Royal College of Obstetricians and Gynaecologists.
Given the benefits to most newborns and concordant with other professional organizations, the American College of Obstetricians and Gynecologists (ACOG) now recommends a delay in umbilical cord clamping for 30–60 seconds after birth in vigorous term and preterm infants.
What cannot be understated however, is the importance of the word “vigorous.”
In the most simple terms, to describe a newborn as vigorous means, the baby is doing well. More specifically, it means the baby has a strong respiratory effort, cry, good muscle tone, and a heart rate greater than 100 beats per minute. This is the case for about 90% of newborns.
However, about 10% are non-vigorous: they have depressed respiration, depressed muscle tone, and a heart rate less than 100 beats per minute. They need help transitioning to life outside the womb. Namely they need assistance to initiate breathing, though 1% of those may require intensive resuscitation efforts.
This means, delayed cord clamping may need to be re-considered if the baby is not doing well. There are more important priorities, like getting the baby breathing.
The other governing organizations mentioned in this post, have caveats mentioned in their recommendations very similar to that of ACOGs.
Going back to our patient, suffice it to say that both baby and mom were having some significant problems. It would have been unwise to allow for delayed cord clamping. Furthermore, while it stands to reason that when less blood is in the umbilical cord it will have less coloration — I’m not certain, that within the time frame of the recommended time delay for cord clamping, that the cord would have been completely white.
Perhaps more concerning is our tendency as humans to think that if a little of something is good, then a lot of it must be better. The concept of delayed cord clamping has been taken to the extreme with a resurgence in interest among certain groups in what is called a lotus birth. A lotus birth (or umbilical cord nonseverance — UCNS) is the practice of leaving the umbilical cord uncut after childbirth, so that the baby is left attached to the placenta until the cord naturally separates at the belly button. This usually occurs within 3–10 days after birth. This apparently involves a special bag or bowl to carry the placenta around in. Just the thing for your baby registry.
Please don’t do this.
There is NO science or data to support the benefit of such a practice. And it carries with it significant risk. The placenta, at this point, is literally a dying, rotting organ. It is a PERFECT setup for infection, and this infection can pass to the baby. In all other aspects of medicine, if there is a dying/rotting/infected organ or appendage, we move to get rid of it. We don’t leave it attached for spiritual reasons. I’m not knocking anyone’s spirituality, but this risky practice has already been the cause of neonatal death.
And it’s fucking gross.
It is wonderful to be an informed patient. But please understand, especially in the peripartum period, all of the healthcare professionals want to do what is best for you and the baby. This might mean a different result or practice than what you’ve read on the interwebs, or what Karen told you is the cutting edge way to ensure your baby is destined for a Harvard MBA while simultaneously curing cancer and leading the NBA in points per game.
Trust us: it brings us no pleasure to deviate from your birth plan. But sometimes, when your safety or your baby’s is at stake, that’s exactly what needs to happen.
This article was originally published on