The Accuracy Of Your Next Mammogram Might Be Compromised By Your Tattoos
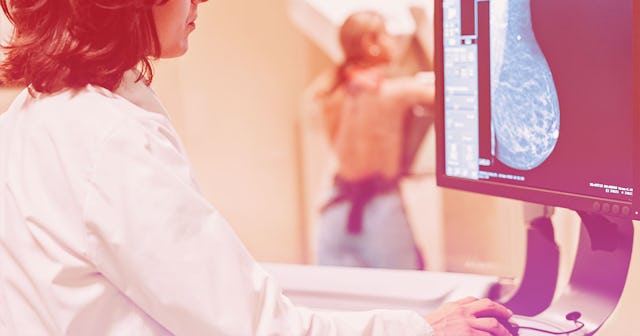
We’ve heard about the importance of mammograms for years. Early detection of breast cancer saves lives, right? So you schedule your mammogram, only to learn that there some troublesome areas that need further investigating. Before you freak out, you might want to consider that your tattoo, or tattoos, may impact your mammogram results.
Forty-six percent of Americans surveyed have at least one tattoo. Perhaps you are among them. Apparently your ink can potentially cause issues with your mammogram. Scary Mommy checked in with Dr. Anjali Malik, a breast radiologist, on everything we need to know about having tattoos and getting a mammogram.
First, it can’t be stressed enough to get your mammogram. Yes, many people pushed off annual exams and appointments because of the pandemic, which unfortunately leaves people vulnerable to more tragic and harder to treat diseases. If you’ve been putting off your mammogram, get it on your schedule ASAP. Dr. Malik shares, “Annual mammograms starting at age 40 for average risk women offers a 40% mortality reduction.” Yes, you read that correctly. Forty percent.
Now, let’s talk about your tattoos. Whether you got something trendy in your twenties or more recently got inked, you need to be aware of the effect your tattoos might have on your breast scans. Dr. Malik says, “The ink from tattoos is drained by our lymphatic system (think of it as the body’s water filter), and can cause calcifications in the lymph nodes through which it is drained.” This means that your tattoo can “affect a mammogram by showing up in the lymph nodes in the axilla (underarm) or within the breast.”
When the radiologist reads your mammogram, they need to know you have tattoos because “calcified lymph nodes can also be seen in metastatic cancers such as ovarian and colon.” Giving the technologist a heads up that you have tattoos can “prevent an unnecessary callback.”
Does it matter where the tattoo is located, how many a patient has, or the type of ink used in the tattoo? Dr. Malik says, “The axillary lymph nodes drain the same side upper extremity (arm, hand) and trunk—upper back and chest. I have seen calcified lymph nodes from large tattoos in any of these areas.”
Another issue, that Scary Mommy has reported on in the past, is the COVID-19 vaccine and mammography. Dr. Malik concurs that the vaccine can “cause same side lymph node swelling.” However, this “usually dissipates 6 weeks after the second or final shot.” This doesn’t mean you should skip the vaccine. Rather, if you’ve had the vaccine recently, ask your doctor when you should schedule your mammogram and alert the technologist of when you had your last shot.
Besides tattoos, other substances can cause false mammogram readings. Dr. Malik says that “deodorant and lotions can layer on the skin and mimic calcifications.” She notes that this is usually more problematic for 2D mammography, but even if you’re getting a 3D, it’s recommended not to wear lotion or deodorant to your appointment.
andresr/Getty
As a breast cancer patient, I’m an advocate of self-breast exams. Twice, I found my cancerous mass by self-exam, since I was considered too young (and not high risk enough) for a mammogram. Dr. Malik shares that if you do a self-exam and find a lump, don’t freak out because “most palpable abnormalities found by women on their self exams are cyclic changes.” She wants us to do our self exams in mid-cycle “because that is when our hormones have the least impact on our breasts.” If you feel something, wait out your full cycle. If the area of concern “decreases or resolves, it was a cyclic change.” If it “grows or persists,” see your doctor.
Keep in mind that breast cancer isn’t always palpable, thus the need for routine mammograms. When you do a self-exam, you need to feel and look. When you look at your breasts head-on (in a mirror) and with your arms above your head, you need to keep an eye out for “dimpling, puckering, or bulging of the skin.” Also check your nipples. If either have “changed position” or “inverted,” that’s cause for concern. Additionally, check for any “redness, soreness, rash, or swelling.”
As a two-time breast cancer survivor, my philosophy is “better safe than sorry.” Report issues to your doctor, even if you don’t have a family history of breast cancer, even if you are young, even if you aren’t positive for the BRCA1 or BRCA2 genes, and even if you don’t have other common breast cancer risk factors. According to the CDC, common factors include drinking alcohol, being fifty or older, never giving birth or breastfeeding, and having dense breast tissue.
If you find a mass, don’t try to self-diagnose online. There are many types of breast masses, and it’s best just to consult with your doctor to see what steps should be taken next. Each patient is different, and we need to not rely on the “experts” (ahem, strangers) on the internet to guide us on our health journey.
Another thing you can do? When possible, have conversations with biological relatives about their health and what they know about other relatives, particularly if they are deceased or estranged. Dr. Malik says, “I stress the importance of knowing our family history, not just of breast cancer, but of all cancers, as these can impact breast cancer risk.” These include ovarian, colon, pancreatic, prostate cancers, as well as melanoma. She also wants us to ask our doctor about “risk assessment” by the time we are thirty, which helps “determine screening protocols.”
Yes, tattoos can cause an issue on mammograms, so can the COVID-19 vaccine, as can your favorite deodorant and lotion, but don’t use these as an excuse. Do your self-exams and schedule your mammogram. You are your best health advocate.
This article was originally published on