A Pediatric Disease Expert Weighs In On The New Inflammatory Condition Linked To COVID-19
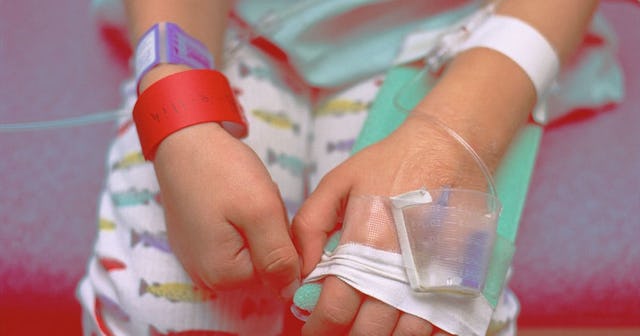
As the COVID-19 pandemic has unfolded, one of the slightly more reassuring aspects of it for parents has been that, for the most part, the virus doesn’t affect kids as severely as adults. Yes, kids can catch the virus and spread it to others, but with some exceptions, most children who contract it survive and generally don’t become ill enough to be hospitalized.
But this novel coronavirus is a brand new virus, and the resulting disease of COVID-19 is a brand new disease, and we are still learning the different ways the virus may affect us, including children. And that’s where things get a little more concerning—and downright frightening, if you ask me.
Over the past few weeks, a new condition called “pediatric multisystem inflammatory syndrome” has emerged. First seen in parts of Europe, there have been about 100 reported cases of it in New York state. 14 other states have reported cases as well. Tragically, three children have died in New York from this syndrome.
This is absolutely awful and extremely worrisome.
The condition, which causes inflammatory symptoms in children—such as fever, rash, swollen lymph nodes, stomach pain, and heart issues—has been linked to COVID-19, because most of children who have it have either tested positive for the virus, or positive for antibodies.
“The majority of patients who have presented with this syndrome have tested positive for SARS-COV-2 or corresponding antibodies,” explains a May 6, 2020 memo from the New York State Department of Health. “Some tested positive on diagnostic, molecular testing for SARS-COV-2, others were positive on serological testing for corresponding antibodies.”
One way that experts are describing “pediatric multisystem inflammatory syndrome” is that it is similar in ways to Kawasaki disease, another condition that causes inflammatory symptoms, as well as toxic shock syndrome. At the same time, as The New York Times, points out, this new condition isn’t exactly the same as Kawasaki disease, or anything anyone has seen before — and experts are still learning how it affects children, along with the best way to treat it.
I don’t know about you, but the emergence of this new syndrome has definitely been keeping me up at night (not that I’ve exactly slept well since this pandemic began!). I am in New York and live up the road from a hospital treating quite a few children with this syndrome. To say I feel unsettled is an understatement.
But they say that knowledge is power, and one of the ways for us to get a handle on things as scary as this is to learn everything we can about it. To that end, we at Scary Mommy interviewed Moshe Arditi, MD, a professor of pediatrics and director of the Division of Pediatric Infectious Diseases at Cedars Sinai Medical Center. Dr. Arditi also happens to be an expert on Kawasaki disease, and has spent much of his career investigating the disease.
Dr. Arditi answered some of our most pressing questions about this new inflammatory syndrome, its links to Kawasaki disease, and more.
How does this new inflammatory syndrome compare to Kawasaki disease? What symptoms does it have in common and what are different?
Interestingly, although Dr. Arditi agrees that “pediatric multisystem inflammatory syndrome” (he refers to it as “Pediatric COVID-19- associated Multisystem Inflammatory Syndrome,” or “PCMIS” here) shares symptoms in common with Kawasaki disease, he wants to be clear that they are not the same thing.
“At this early stages of our understanding of this new disease, I believe that the data we have so far strongly suggests that PCMIS is not a manifestation of Kawasaki Disease or Kawasaki Disease shock syndrome, and the use of Kawasaki Disease is a misnomer in this new disease,” Dr. Arditi explains.
As he describes it, the patients with this new inflammatory condition are presenting with features of both Kawasaki disease and toxic shock syndrome. “Both of these conditions are uncommon and affect the blood vessels and cause inflammation of blood vessels, called vasculitis,” he explains.
Symptoms of Kawasaki disease, including conjunctivitis, red lips, red tongue, and rash, are being seen with this new condition. But there are some key differences between Kawasaki disease and this new syndrome, according to Dr. Arditi.
“It soon became clear that these children appeared to have a new febrile illness involving systemic hyperinflammation, multi-organ involvement, severe abdominal pain and diarrhea, very prominent cardiac shock with severe myocardial dysfunction, as well as kidney injury,” Dr. Arditi clarified. “None of these are seen in typical Kawasaki Disease, but they are hallmark of toxic shock syndrome.”
FS Productions/Getty
In fact, he says, many of the symptoms these children are experiencing are similar to those experienced by adults who have COVID.
“The overall clinical picture of children with this new entity is similar in many respects to the later phase of adult COVID-19 infection that is characterized by vasculitis, cytokine storm, hyperinflammation, multi-organ injury, often including severe myocarditis, diarrhea and acute kidney injury and laboratory features of TSS and/or MAS,” said Dr. Arditi.
Why do you think this new inflammatory condition seems to be affecting children only now, several months into the pandemic?
Researchers are still looking into this question, said Dr. Arditi. And right now, they still just don’t know.
In some cases, he says, children are testing positive for COVID-19 and seem to be in the middle of an infection. “In these children it is possible that the active viral infection is triggering a cytokine storm and toxic shock that may be due to some unidentified toxins in the virus,” Dr. Arditi explained.
But many of the children with this syndrome are not currently positive for the novel coronavirus, or SARS-CoV-2, and instead are found to have antibodies for it, says Dr. Arditi. This suggests, he says, “that this hyperinflammatory syndrome is occurring 10-14 or more days after the initial infection and that the antibodies may be playing a role in this disease, perhaps through a mechanism that may involve immune enhancement.”
“In brief, it is very mysterious why this new syndrome occurs in children who haven’t manifested the early stages of COVID-19,” explains Dr. Arditi. But he reassures us that “intense research efforts are underway” to get to the bottom of this all. Thank goodness.
What should worried parents keep in mind about children and COVID-19, and this particular new development?
So here’s the burning question: how worried should parents be?
“While this new string of illness is troublesome, I want to remind parents the number of COVID-19 cases among children overall remains very small and while some children and infants have been sick with COVID-19, adults make up 98% of the known cases to date and only up to 2% of the COVID-19 cases are among children,” Dr. Arditi assures.
This new inflammatory syndrome is still considered a rare disease, he explains further.
And what should parents do in the meantime?
“Parents should be reassured that children are unlikely to be seriously ill with COVID-19, and I urge parents not to panic, but instead, remain vigilant and call the doctor if their child presents with fever, rash, or any unusual or new symptoms,” he says.
Phew. I’m definitely going to take Dr. Arditi’s smart advice and remain vigilant – and definitely call my doctor if my kids get any concerning symptoms at all. The part about “trying not to panic” is going to be a little easier said than done, but I’ll work on that too. We all should be working a little harder at that, huh?
The bottom line, though, is that SARS-CoV-2 is a brand new virus and there is just so much we don’t know about it yet. I think we all need to do our best to remain patient, let doctors and researchers do their thing, keep ourselves as up-to-date and informed as possible – and do everything in our power to keep our kiddos healthy and safe in the meantime.
Information about COVID-19 is rapidly changing, and Scary Mommy is committed to providing the most recent data in our coverage. With news being updated so frequently, some of the information in this story may have changed after publication. For this reason, we are encouraging readers to use online resources from local public health departments, the Centers for Disease Control, and the World Health Organization to remain as informed as possible.
This article was originally published on