I Had A Hysterectomy — Here's What You Can Expect
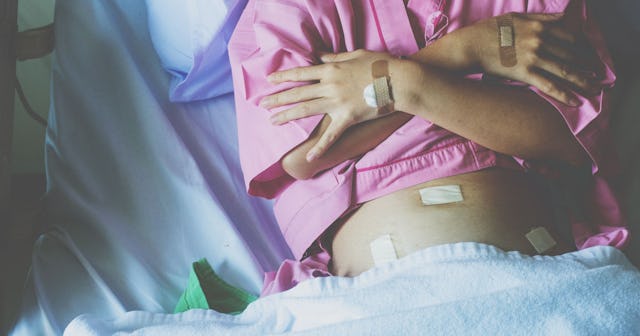
In the days leading up to my hysterectomy, I was scared. I’d had surgeries before, including a myomectomy to remove over eighteen fibroids. But something about this surgery was different. My surgery was a robotic laparoscopic hysterectomy. My uterus, cervix, and fallopian tubes were removed, leaving my ovaries intact.
After c-sections, hysterectomies are the second most common surgery of women in the United States and over 600,000 women get hysterectomies a year. Of course, I had the typical fears: Would my hormones shift so drastically? What would my sex life be like afterward? How would my recovery go? Thankfully, my doctor was amazing. I felt well prepared before, during, and after surgery. Here’s what I learned along the way.
The week before my surgery, I was handed a shiny white folder from Dr. N, an OB/GYN and oncology specialist. In the packet were recommendations for planning for surgery, pre-op instructions, and post-surgery details, along with directions to the hospital. I leaned into all of the instructions provided.
I became more and more nervous as my surgery date neared. I am a planner — I like to know when, how, and why things are happening — so planning for my hysterectomy was no different. I wanted as much control over the situation as possible. This is what I found helpful to have in place before I went in for my operation.
- My surgery was outpatient. I expected to be discharged before dinnertime. My wife took responsibility for all of the coordination for our kids from school pick up to dinner. I also left her a note via email, which I had little faith she’d remember to look at, for reminders. I hoped she would not forget them at school, but once I was wheeled into the operating room, all that would be out of my control.
- I picked up all medications recommended by my doctor before surgery. Tylenol and Aleve were my two best friends in the days following surgery. I also picked up a bottle of Hibiclens, an antibacterial/antimicrobial skin cleanser, that I had been instructed to use the night before surgery.
- I maintained a pretty simple diet; for me, it was an important part of the planning phase of my surgery. I tried to steer clear of sugar, dairy, and gas-inducing foods a week before my surgery. I stayed hydrated and drank water … all the water … all of the time.
- Find a few meditations to listen to leading up to and while waiting for surgery to begin. I did not do this, but I wish I had, because I felt so much anxiety that I even yelled at my wife while looking for parking before my surgery. I nag, sure, but yelling at her happens once in a blue moon. I knew my anxiety had gotten the best of me in those moments.
The day before my surgery, Dr. N recommended that I have only clear liquids. The surgery, if all went as planned, was outpatient. I’d arrive, have my surgery, go into observation, and, discharged the same day. As fate would have it, my surgery started late. They chose to keep me overnight for one night, as not to discharge me late in the evening.
After my surgery, Dr. N recommended that I not consume “gas-producing foods,” like broccoli, cabbage, and beans, or greasy, fried foods, dairy, oatmeal, and high-fat foods. So, all of the stuff I like. I chose to alter the post-op food recommendations and stopped all of these foods one week before my surgery. I think this helped me during my recovery. Gas, as anyone who has had surgery knows, is part of the process, part of the road to recovery.
I am grateful that my body heals the way that it does. I have had enough surgeries to know what to expect after surgery from my body. I needed frequent reminders to follow the doctor’s orders:
- Not to drive one week after surgery, and especially not while on narcotics. Oxycodone was prescribed after my surgery. I never picked it up from the pharmacy, because the pain was bearable for me. As long as I stuck to the every-four-hour Aleve/Tylenol combo, I could manage my pain.
- No lifting. It’s easier said than done, especially when you have kids. But if you want to recovery quicker and avoid complications, don’t lift anything over ten pounds for six weeks after surgery. Not even if it feels like you can. No lifting is important because the last thing anyone wants is another surgery, which could happen if you develop an incisional hernia, which accounts for 15-20% of all abdominal hernias.
- No exercising — which was admittedly not a problem for me before surgery. Walking, however, is something I began doing four hours after my surgery. It’s important to do to avoid blood clots, to move the gas around, and to help speed up your recovery.
- Vaginal spotting is a normal part of the healing process post-hysterectomy. This is something I don’t remember the doctors preparing me for. While for me there was only spotting, in some of the Facebook groups I am in, women reported filling up pads post-surgery. The vaginal spotting should end in the days following surgery and should not fill up a pad. If it does, contact your doctor.
- If your ovaries are left, you won’t get your period, but you will still get all of the period (and PMS) related symptoms you had prior to the hysterectomy. It’s super annoying — but hey, no bleeding, so there’s that.
- Lay down. But for your sake and your recovery, lay down. Rest. Sit on the couch if you can. Lay on the couch. Stay in bed and rest. Even if you feel energetic after the first day or two, the surge is not going to last, and if you take it too far — walk too much, run errands, clean parts of your house — you’ll regret it later.
- Take those stool softeners; you will thank your future self. Gas is real and they enlarge your abdomen during surgery to get a better view of what they are doing, adding fuel to the fire. It can be challenging to manage and painful. You don’t need to add pushing and straining through constipation to the mix.
Deciding to get a hysterectomy is not an easy one. It takes time to come to terms with what it means for you to, at minimum, decide to remove your uterus. Everyone’s body is different, everyone’s recovery from a hysterectomy will be different, and you will make the decision that is best for you. Being well informed about your options, building the right medical team, and pacing yourself at your own time, will help you to decide.