My Traumatic Birth Story: Surviving Preeclampsia And Making The Decision To Be 'One And Done'
On a hot summer evening in July 2019, I was in my eighth month of pregnancy, at a wedding on a farm in the outskirts of town. I asked my husband Pierce to accompany me to a shaded patio lounge chair I spotted near the edge of the property, which is where I spent the majority of the reception. Someone snapped a Polaroid as they walked past us, and I was sight to see, a hugely pregnant woman with her feet up, being fanned by her doting partner as the party raged on around us. I remember fantasizing about lying down on the top of an old wooden picnic table in the distance; I just desperately wanted to sleep. I assumed this was a normal symptom of pregnancy and typical for the third trimester. I would soon find out that this level of exhaustion was the first sign that I was very sick and my pregnancy was endangering my life.
Courtesy of Jessica Myhre
My pregnancy up to this point had been somewhat eventful. My 20 week scan revealed that my daughter had a marginal cord insertion, which occurs when the umbilical cord attaches on the side of the placenta instead of in the middle. This can lead to restricted fetal development and growth as well as other complications. I was also informed that her kidneys had not developed at the proper rate and there may be issues related to her urinary tract when she is born. She was clocking in at the 20th percentile, which was decent but on the low end of the growth spectrum. They told me I would be getting monthly ultrasounds to keep an eye on the abnormalities and my pregnancy was considered high risk at that point. There was no root cause specified for any of these issues, and they assured me that they were all common and just needed to be watched a little more closely.
On top of all of this, I have spent a lifetime suffering from general anxiety disorder. From the moment I became pregnant, I checked an online “miscarriage likelihood calculator” at least once a day. I obsessed over every little thing, I avoided any and all foods that would affect my pregnancy and I was incredibly rigid with everything from the bath temperature to limiting myself to 1.5 cups of coffee each day — down to the milligram. The pressure of keeping this child safe ramped up my already intense anxiety to an extent that I lacked the tools to cope with.
A week after the farm wedding, as I prepared for my scheduled 36 week ultrasound, I spent a Sunday night sobbing in Pierce’s arms. I begged him not to let me die, I told him I was terrified to give birth because I may never see him again. I told him I was sorry that if I die I won’t be able to help him parent our daughter. My eyes were puffy from crying all night as I entered the routine appointment, I was shaking and could barely stand. For no reason aside from what I would later call my first dose of motherly intuition, I was overtaken with a fear that I had never experienced: a deep, unrelenting fear of death. When the ultrasound tech hurried out of the room mid-scan to consult with the physician, my heart sank and my anxiety grew into a state of shock.
Courtesy of Jessica Myhre
The doctor rushed in, a woman I had grown to know and love since my 20 week scan. With concerned eyes but a calming, sisterly demeanor, she revealed to me that my blood pressure repeatedly measured at a dangerously high rate, nearing 200/120 at one point (120/80 is considered normal). She also told me that my daughter’s growth had dropped from the 20th percentile all the way down to the 2nd. Visibly fighting back tears, she told me, “You need to head to labor and delivery now. Do not stop at home, do not wait, it’s time to go to the hospital. You will not be leaving without a baby.”
Pierce was dressed for work, he had planned on heading there after our appointment. We both had coffees in our travel thermoses, his lunch was packed and waiting for him on the front seat. Our days were supposed to continue as normal. We drove separately as we had for every routine appointment in the months before. Luckily, our go-bag was packed and in the trunk of my car, something I can thank my anxiety for repeatedly reminding me to do and eventually causing me to complete around the 30 week mark. I spent the following six weeks adding to and perfecting it, so we were pretty set when they wheeled me into the triage wing of labor and delivery.
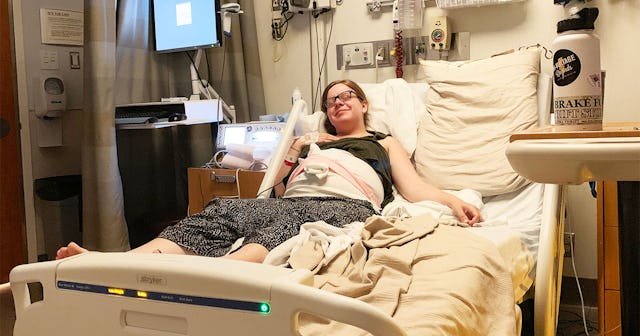
Within an hour they had given me a steroid shot in my back. They told me it was to help the baby’s lungs develop because she will be born prematurely. I was diagnosed with preeclampsia and was told it was very severe. They placed me on IV medication to lower my blood pressure and I soon started to feel better than I had in weeks. My high blood pressure snuck in so discreetly; in the appointment a month before, it was still considered normal but higher than my usual. The month before that it was considered low but slightly higher than the visit prior. I don’t know how long it had been creeping up, but when it lowered I felt a sense of calm wash over me.
Courtesy of Jessica Myhre
I was transferred into a room and the next 24 hours was spent monitoring my blood pressure, keeping tabs on our baby’s heart rate, and deciding on a plan of action for us. I received a second steroid shot the next day for her lung development and was given lots of conflicting information from various members of my care team. Some doctors told me I would be induced later that day, a nurse told me I’d likely be sent home and told to return for an induction on the weekend. As the second day progressed, it became clear that I was no longer responding to the blood pressure medication and my dosage had to be continually raised. They finally told me I would not be going home, and my induction would begin on day three of my hospitalization.
On the third day, my blood pressure was out of control again. I hadn’t slept more than two hours at a time since my arrival as I was hooked up to a blood pressure cuff that checked me every couple of hours. I was placed on magnesium as a last ditch effort to regulate it while also being administered Cervidil in order to start the process of induction. As my contractions began, my blood pressure was a constant battle for the doctors and nurses and our daughter’s heart rate was starting to be affected by the many medications I was on. I begged for a C-section, I wanted this to be over. I was shaking uncontrollably by day four and they had thrown so many drugs my way for the pain and discomfort that I lost my grip on reality and could no longer communicate via phone with friends and family. By the time I was finally dilated enough to go to the delivery room, I could barely keep my eyes open long enough to be given the epidural.
The delivery room was large, and in my memory resembled the inside of a spaceship. There were at least a dozen people in there tending to me, along with Pierce and my mom. They knew our daughter would need assistance upon delivery so the whole NICU team was there, they set up a warming bed for her to help get her up to temperature, and everyone was gearing up to take care of a medically fragile and premature newborn. It took me hours to push, my body had no strength left and mentally I was floating in and out of consciousness. I was later told that I was very close to having a stroke at various times during my stay at the hospital and they opted for a natural delivery because I may not have survived a C-section.
Courtesy of Jessica Myhre
Penelope was born at 1:44AM on the fifth day, weighing 4lbs 11oz. She needed some help regulating her body temperature, but I was able to do skin-to-skin and nurse her immediately. Pierce held her under a warming light as I was stitched up. I believe I fell asleep soon after. We were discharged a day later as she was given a clean bill of health. Unfortunately, we would return to the children’s hospital within a couple days due to jaundice — and that’s when we were alerted to some other conditions she had that they had missed in the initial newborn assessment. She had a heart condition and was suffering from bradycardia and hypothermia. Her lungs were cloudy, she wasn’t getting enough nutrients while breastfeeding, and she was struggling to stay alive. The nurses told me she should have been placed in the NICU and never should have been sent home.
As they worked to stabilize my newborn baby, my vision was tunneling and there were streaks of light in my peripherals. I had to have the blinds of her hospital room closed at all times. I wasn’t sleeping, I wasn’t eating, I slept next to her bilirubin lights and held her tiny hand as I wept for hours at a time. I was physically healing from delivery, my hormones were all over the place, and I was completely traumatized by the week before. My head ached from crying and I silently ignored my own worsening health. When I finally left her side to get a blood pressure monitor as I had been advised to do when I was discharged, it was sky high yet again. My mom took me from Penny’s bedside to the emergency room entrance and I was admitted with postpartum preeclampsia. They put me back on intravenous medication, prescribed me with more to take at home, and I left as quickly as I could to get back to my daughter.
Penelope’s medical issues were addressed but still to this day, years later, have to be closely monitored. My preeclampsia took about four months to go away, and I have been left with a potential in the future of high blood pressure, cardiac issues, and long term eye damage. That experience left us both with long term consequences physically, and for me, mentally. The trauma of my birth experience and the repercussions on my daughter haunted me for months, causing dangerous intrusive thoughts, crippling fears of sickness and death, and ultimately I was diagnosed with PTSD and postpartum anxiety.
Courtesy of Jessica Myhre
I shared my birth story to those close to me, I was open about seeing a therapist and spoke about how emotionally disturbed I was by being so close to death while trying to bring life into this world. Yet, without fail, as soon as a week after we finally arrived back home from the children’s hospital, people started asking when we were planning on baby #2. They told us that preeclampsia wasn’t guaranteed to happen again, that it was a fluke and no reason to decide not to have another child. I was already considering being one and done by the time we left the hospital but I kept my mind open. When COVID-19 hit six months into my journey into motherhood, my stance was cemented. There was no way I could handle getting pregnant again. I was firmly one and done — and it was not a very popular decision with our friends and family.
That is how we came up with Only You: A One and Done Podcast. Pierce and I created this show during quarantine and found a community of folks who have decided to only have one child for a wide array of reasons. Some of them suffered infertility or loss, others experienced a similar birth trauma. We have folks write in who simply could not handle the emotional weight of becoming parents again, or their relationships couldn’t handle it, or they couldn’t afford another financially. Having a child is such a personal choice yet in our society it is treated as a group decision. I am now spending my time advocating for other one and done parents, whether by choice or by circumstance, and using my own experience to shed light on the varying paths others have taken to get here.
Having my daughter was the hardest thing I have ever done, but I don’t regret a single second of it because it gave me her. I will not tempt fate with another go at pregnancy, and I am very satisfied and fulfilled by the life we have with just the three of us. This is our story and it is the only birth story I will ever write. The trauma, profound love, and visceral memories associated with it are mine to carry and I want to share so that others can feel validated in their stories as well, wherever they may lead.