What A Swollen Foot Taught Me About Listening To My Instincts
I have followed every doctor’s order and I have received good medical reports every time I leave my fortnightly appointments (yes, you have a lot of appointments when you carry multiples). My fetal expert doctor tells me my babies are growing, their blood flows are good; Baby #2 has a missing vessel, that’s why it weighs less but there’s no need to panic, they are still growing well. I have obeyed every warning about overdoing doing it and accepted I need to be signed off work to keep my babies healthy and myself well to avoid a very premature labor.
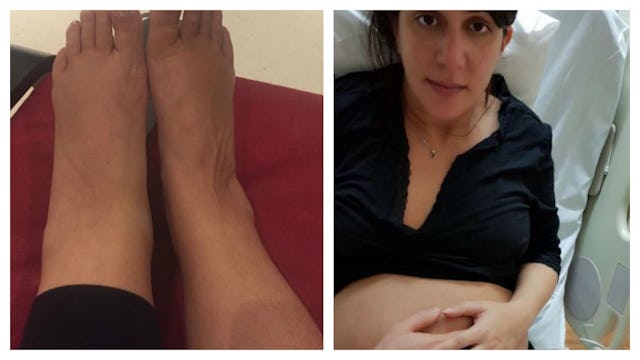
Last Saturday, I started to feel unwell. It started with swollen feet, one particular foot looked like it had elephantitis. I have included a visual representation, for your comedy value, which my husband, Simon, compares to a hoof.
Marina Koniotou Innes
My other symptoms included a headache, exhaustion and fever. Every day for the past week felt like Groundhog Day: I would blast the A/C, Simon would come home and switch it off, and the bickering would start. He had just recovered from a chest infection but I was still hugely annoyed; it’s not him who is carrying three babies the size of cabbages. He could not function in a room of 19 degrees Celsius and just increasing it by one degree would give me the sweats. I decided that I needed to see the doctor and I also requested to bring forward my steroid jab for the development of the babies’ lungs in case they came early.
Something didn’t feel right.
The following day we drove to the hospital and I was given an internal examination of my cervix. I was told it had began to open by 1.5mm and that I would not be going home. I tried not to panic and held back the tears. I told myself that would make the situation worse and undue stress could trigger the labor. I told myself this would not be so bad, all I had to do was rest and keep them in – no pressure, hey. That’s been the catchphrase of my triplet pregnancy, “Keep them cooking / keep them in for as long as possible.” I can assure you, I’m doing all that I can.
On my second day at the hospital, the nurse told me I would have a cardiotocography (CTG) when I felt any cramps or contractions. I was feeling mostly fine, I had some very mild cramps and decided to buzz the nurse. I explained they were mild, but if she wanted some baseline information she may as well do a CTG. We both didn’t take it too seriously, it felt like mild menstrual cramps and not particularly unpleasant.
The next sequence of events that unfolded was beyond traumatic and a complete nightmare. They were giving me a CTG, the belts were ridiculously tight, the nurses were making a huge fuss and apparently telling me my contractions were strong. I kept asking them if they were sure, as it just felt like my three beautiful babies were having a rave, just bashing out some shapes, “big box, little box,” if you know what I mean. Apparently not – this was SERIOUS.
I was told I needed drugs to delay the contractions, especially as the steroids did not have enough time to progress the development of the babies’ lungs. They reiterated this still might not stop the contractions; I kept trying to get my head around all the information. I was told to sign paperwork to give consent that two of our babies would stay at the hospital and the other had to go elsewhere since they didn’t have a third bed. It was 3 a.m. and I did not want to wake Simon for a false alarm, but things were getting serious. I made a pre-decision as I didn’t want to call him in a fluster and in case I couldn’t get through – all that was left was to make sure we were on the same page about what happens next.
Having explained everything, Simon 100% agreed — we would not allow them to be separated. My delivery doctor walked out the room, the two midwives echoed my worries. “It’s not a good idea to separate them, one may need more support than the other” and all I could think was how would I divide my time travelling between two hospitals and after giving birth by a C-section. There were so many unanswered questions, I guess the look on my face said it all.
The delivery doctor told me in a very matter of fact way that I would not breastfeed – it was as though she could read my mind. It was all getting to me, during the septum examination I asked them to stop and the doctor screamed that she would not stop. I wondered if this firm approach can be helpful during a delivery, but deep down it all felt a bit feral and unnatural. It kept playing on mind that she told me she had visitors staying for the F1 weekend and she was exhausted. These were warning signs not to be ignored, especially as there is me and another three to take care of now.
We had made our first family decision and I was to be transferred to a specialist government hospital if they had three available beds. I had heard great things about this hospital and thought this was the best option. Off I went in the ambulance, with Simon to meet me at the new hospital.
On arrival, the doctors started the second round of examinations. It was 6 a.m., I was delirious and I felt like a lab experiment. I wanted to scream and tell them to stop prodding me and taking blood. I don’t want a 16 gauge needle, I have an 18 gauge needle in my right hand and stop blooming examining my cervix – it had been examined four times in less than 48 hours (three times in 4 hours). I was not happy!
I moodily explained, “You already have my information from the other hospital, why are you undertaking these tests again.” It wasn’t their fault and government hospitals, as opposed to a private hospital, follow international protocols and guidelines.
They decided not to administer the drugs to delay the contractions; instead they gave me a scan and they told me these were no longer contractions. They gave me a less sophisticated room than the previous hospital. Coincidentally, my doctor — one of the best doctors in Abu Dhabi — sent a reply to an email I sent her a few days ago. She explained the results of my culture had come back and that I had a common urinary tract infection and needed to share this information with the hospital. And it was as easy as that – it looked like the UTI had triggered off the contractions and to a small degree impacted my cervix.
I’m now halfway through my treatment and finally back home after a very long and an awful week. I’ve learned that not every doctor is adept in triplet pregnancy and others absolutely love the challenge of a high-risk pregnancy. A mother’s gut instinct is strong. I could be at the hospital right now visiting either two or one of my babies across two separate hospitals in NICU and who knows how long they would have needed to stay in NICU. Instead, I’m resting at home and grateful for each and every extra day these sprogadoos get to grow inside of me. My new goal is to make it to Monday to bring me to week 30.
Pregnant ladies, a word of advice, here are some of the symptoms of a UTI:
– Pain or burning when urinating
– More frequent urination
– Feeling of urgency when urinating
– Blood/mucus in urine
– Cramps/pain in lower abdomen
– Pain during sexual intercourse
– Chills/fever
– Incontinence
As you know from my experience, a UTI can trigger early contractions so be sure to see a doctor immediately. If the UTI goes untreated, it could lead to a kidney infection, which could cause early labor and low birth weight. But according to the American Pregnancy Association, if your doctor treats a urinary tract infection early and properly, the UTI will not cause harm to your baby.
It is important to note that if the infection has spread to your kidneys, you can get seriously ill and symptoms may include fever; pain in your back, abdomen and pelvis; or diarrhea, nausea, and vomiting.
I have every intention of bringing you a fun, witty blog, but that would not be a true reflection of what it’s really like to be pregnant with triplets. It’s unpredictable, uncomfortable and like nothing else I have experienced.
This article was originally published on