Your Go-To Guide To Plan B: What To Expect From This Emergency Contraceptive
From weight limit to side effects, here's everything you need to know.
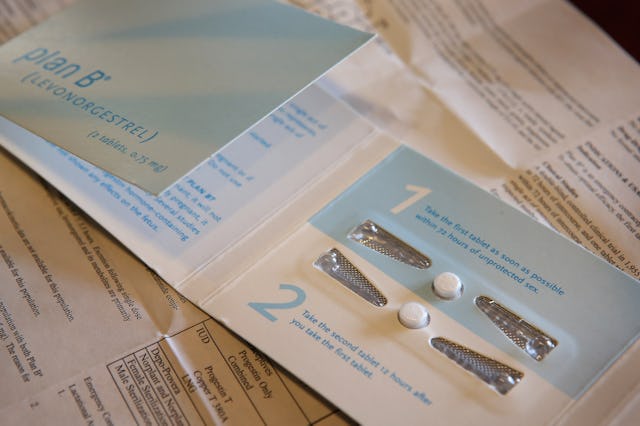
Living in a post-Roe v. Wade world is terrifying; make no mistake about that. However, one thing you don't need to worry about (yet) is the emergency contraceptive known as Plan B. While you shouldn’t use Plan B as regular birth control, it's a highly effective and useful option immediately after having unprotected sex. You can pick it up without a prescription, order from almost any pharmacy or big box retailer with an online presence, and you don't even need to do it yourself — you can send your sexual partner, bestie, or auntie to pick it up, too. Now that access to safe, legal abortions is off the table in many states, you need a solid backup plan for any unprotected sex you might have.
But it's important to know what you're putting in your body, how to use it, and how it works. Any time you take a new medicine, you're undoubtedly riddled with questions — even when it's not a medication that has already taken quite a bit of heat. Is it basically the "abortion pill”? Will you need a D&C afterward? Can you still end up pregnant? Will it work on all-sized bodies? And how exactly will you feel after you take Plan B?
Whatever you're wondering, there's an answer available to assuage your curiosity and concerns. And, remember, now is the perfect time to go to your doctor with any more questions.
How does Plan B work?
First things first, Plan B is simply one name brand for a drug called levonorgestrel. Because it's the most popular option with arguably the most name recognition, it also comes with a heftier price tag. However, stores like Walmart, Target, and Amazon sell other brands of levonorgestrel, all with the same or similar reviews.
What is levonorgestrel? Levonorgestrel works by releasing chemicals in your body that keep an egg from fully developing. It can also prevent an egg (that might have already developed) from attaching to your uterus.
"Emergency contraception or 'morning after pills' like Plan B are highly effective at preventing a pregnancy no matter the brand name," shares Colleen Quinlan, Ph.D., an associate professor of nursing at The University of Toledo, board-certified Women's Health Care Nurse Practitioner, and a former clinician at Planned Parenthood of Northwest Ohio. "Most brands use a synthetic hormone to stop your ovaries from releasing an egg (ovulation). If there is sperm in your body but no egg, fertilization cannot take place."
In other words, because levonorgestrel stops an egg from forming or attaching, it's protecting your body from the sperm and the chance of getting pregnant. Since Plan B helps prevent pregnancy, it's not an "abortion pill." Abortion pills end a pregnancy after it's already occurred. Plan B stops pregnancy from occurring.
When should you take Plan B (or similar emergency contraceptive)?
For emergency contraceptives, timing is everything. Plan B is most effective within the first five days (120 hours) after you've had unprotected sex. However, the sooner you take it, the more effective it will be.
"Plan B is 98-99% effective in preventing a pregnancy when taken within 72 hours," explains Quinlan. "Plan B may be taken up to five days after unprotected sex and still be 85-90% effective in preventing a pregnancy. Plan B and other brands are available to buy by both men and women at the pharmacy without a prescription."
How much does a Plan B cost?
According to GoodRx, brand name Plan B ranges from $38 to $50. Generic versions, however, can cost as low as $10, depending on your area, like Take Action, MY Way, EContra EZ, and Opcicon. Prices may vary online and can be bought over the counter.
How often can you take Plan B?
According to Planned Parenthood, you can take Plan B as often as needed. Taking the morning-after pill more than once doesn't ruin its effectiveness or lead to any long-term effects. But it's important to note that it shouldn't be used as a daily contraceptive. Birth control taken before or during sex is much more effective and less expensive.
Can Plan B affect your fertility?
Contrary to popular belief, Plan B or taking Plan B often will not affect fertility. It does not increase your likeliness for miscarriages or harm your chances of becoming pregnant later in life. Plan B has levonorgestrel, which is a progesterone and one of the hormones obstetricians examine during pregnancy to ensure it's at the proper level. The chemicals in Plan B aren't toxic or completely foreing to the body, especially when used correctly.
Does Plan B expire?
Plan B's shelf life is about four years. In other words, if you're adamant you don't want to get pregnant and want to take extra precautions, it wouldn't hurt to have one on "stand-by" for emergencies. That way, as soon as you have an "oops" moment, you know you have an emergency contraceptive that you can take immediately. Once the four years have passed, your best bet is to replace your stock. It appears the most significant risk in taking expired Plan B is that it might lose its efficacy.
Is there a Plan B weight limit?
Not exactly.
"Plan B starts to lose its effectiveness when women weigh more than 165 pounds or have a BMI greater than 25," says Quinlan. "These women should consider taking the brand ELLA, which is available by prescription, as it is more effective in heavier women. It is not harmful for heavier women to take Plan B, and it may still be highly effective at preventing pregnancy, but if available, it is recommended these women consider taking ELLA."
The internet is full of people who will tell you that if you're worried about your weight and Plan B's effectiveness, you can "just take two." While there doesn’t appear to be anything explicitly warning against that, you should always talk to your doctor or pharmacist before taking more medicine than the instructions suggest. This may not warrant a visit, but just a phone call to a doctor with whom you have an already established relationship.
A better option would be to talk to your doctor now, before you need emergency contraception. They can give you the best advice on Plan B and even prescribe ELLA for you to fill and keep safely stored.
Are there any Plan B side effects?
"You may experience nausea or headache after taking Plan B, so it's best to take it with food," says Quinlan. "You may get your next period sooner or later than you expect, but likely within the same week you were due to have it. Your next period may also be lighter or heavier than what is normal for you. Emergency contraceptive pills are not abortion pills. They can do no harm to you or your baby if you are already pregnant when you take it."
Taking a Plan B? It sounds like you'd be fine to work if you need to. Still, you might consider taking the day off work to catch up on your favorite show or listen to a podcast.
Expert Source:
Colleen Quinlan, Ph.D., associate professor of nursing at The University of Toledo, board-certified Women's Health Care Nurse Practitioner, and former clinician at Planned Parenthood of Northwest Ohio
This article was originally published on